Arachnoidalzyste








































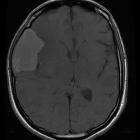
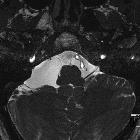



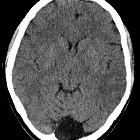
Arachnoid cysts are relatively common benign and asymptomatic lesions occurring in association with the central nervous system, both within the intracranial compartment (most common) as well as within the spinal canal. They are usually located within the subarachnoid space and contain CSF.
On imaging, they are characterized as well circumscribed cysts, with an imperceptible wall, displacing adjacent structures, and following the CSF pattern (hypodense on CT and hyperintense on T2 with FLAIR suppression on MRI). They can also have a remodeling effect on the adjacent bone.
Epidemiology
Arachnoid cysts account for ~1% of all intracranial masses. Although the vast majority are sporadic, they are seen with increased frequency in mucopolysaccharidoses (as are perivascular spaces).
In a retrospective cohort study of 48,417 patients who underwent neuroimaging, arachnoid cysts were identified in 661 patients (1.4%) with a statistically significant male predilection .
Clinical presentation
The majority of arachnoid cysts are small and asymptomatic. Approximately 5% of patients experience symptoms and when symptoms occur, they are usually the result of gradual enlargement resulting in mass effect . This results in either direct neurological dysfunction or distortion of normal CSF pathways resulting in obstructive hydrocephalus . Sellar/suprasellar, quadrigeminal, and cerebellopontine angle arachnoid cysts were more likely to be symptomatic .
Genetics
Arachnoid cysts are almost always sporadic and nonsyndromic, but association with acrocallosal, Aicardi, and Pallister-Hall syndromes have been reported .
Pathology
Arachnoid cysts are thought to arise due to the congenital splitting of the arachnoid layer with accumulation of CSF within this potential space. The cyst wall is comprised of flattened arachnoid cells forming a thin translucent membrane. There is no solid component and no epithelial lining.
Radiographic features
Arachnoid cysts can occur anywhere within the central nervous system, most frequently (50-60%) located in the middle cranial fossa, where they invaginate into and widen the Sylvian fissure. In this location, they can be classified into three types based on their size: see Galassi classification. Of these, Galassi type I is most common accounting for 78% followed by Galassi II and III with 19% and 3% respectively . The retrocerebellar location accounts for 30-40% of arachnoid cysts .
Some locations deserve special mention and separate discussion:
- suprasellar cistern (see suprasellar arachnoid cyst)
- within the ventricles (see intraventricular arachnoid cyst)
- posterior fossa
- cisterna magna (need to be distinguished from a mega cisterna magna)
- cerebellopontine angle (need to be distinguished from an epidermoid cyst)
- spinal canal (see spinal arachnoid cysts)
CT
Arachnoid cysts are extremely well circumscribed, with an imperceptible wall, and displace adjacent structures. When large, and over time, they can exert a remodeling effect on the bone.
CT cisternography (introduction of contrast into the subarachnoid space) demonstrates communication of the cyst with the subarachnoid space. As this communication is slow, the cyst often fills later, and contrast may be seen to pool with it, outlining its dependent portion.
MRI
As they are filled with CSF, it is not surprising that they follow CSF on all sequences, including FLAIR and DWI. This enables them to be distinguished from epidermoid cysts for example. As their wall is very thin it only occasionally can be seen, and displacement of surrounding structures implies their presence. As there is no solid component, no enhancement can be identified.
Phase contrast imaging can also be employed not only to determine if the cyst communicates with the subarachnoid space, but also to identify the location of this communication.
Magnetic resonance cisternography: high resolution sequences such as CISS & FIESTA help to delineate cyst wall and adjacent anatomic structures.
Treatment and prognosis
Arachnoid cysts are benign, and the vast majority remain asymptomatic throughout life. If they are deemed to be causing symptoms, then surgery can be contemplated. This can either take the form of a craniotomy (fenestration or excision) or placement of a cystoperitoneal shunt.
A rare complication is spontaneous rupture in the subdural space .
History and etymology
Richard Bright was the first to describe an arachnoidal cyst in 1831 .
Differential diagnosis
General imaging differential considerations include:
- enlarged CSF space (e.g. mega cisterna magna)
- epidermoid cyst
- often shows a heterogeneous/dirty signal on FLAIR
- restricted diffusion
- more lobulated
- tend to engulf adjacent arteries and cranial nerves
- subdural hygroma/chronic subdural hemorrhage
- do not typically show CSF signal intensity on MRI
- can have an enhancing membrane
- cystic tumors: often will have a solid/enhancing component and be intra-axial
- non-neoplastic cysts
- neurenteric cyst
- neuroglial cyst
- porencephalic cyst
- often follow a history of trauma or stroke
- surrounded by gliotic brain
- tumefactive perivascular spaces, especially anterior temporal lobe perivascular spaces
- neurocysticercosis
- small cyst
- usually multiple when in the subarachnoid space
See also
Siehe auch:
- Mega Cisterna magna
- subdurales Hygrom
- Arachnoidalzysten der hinteren Schädelgrube
- Pilozytisches Astrozytom
- subdurales Hämatom
- Neurozystizerkose
- Wurzeltaschenzysten
- neuroglial cyst
- Hämangioblastom
- spinale Arachnoidalzyste
- epidermale Inklusionszyste
- Dandy-Walker-Syndrom
- neuroenterische Zyste
- Galassi classification of arachnoid cysts
- Porenzephalie
- fetal arachnoid cyst
- Orbitadysplasie
- temporal arachnoid cyst
- frontale Arachnoidalzyste
- spontaneous rupture of a subarachnoid cyst
und weiter:
- Rathke Zyste
- Tuberöse Sklerose
- Pinealiszyste
- Empty-Sella-Syndrom
- intrakranielle Epidermoidzyste
- Tumor Kleinhirnbrückenwinkel
- Dandy-Walker continuum
- subarachnoid space
- ependymal cyst
- subdurales Empyem
- Myelomeningozele
- semi-lobar holoprosencephaly
- intraventricular epidermoid
- Dysgenesie des Corpus callosum
- intraventrikuläre Arachnoidalzyste
- differential diagnosis of intracranial cysts in the perinatal period
- diffusionsgewichtete Bildgebung
- intraventrikuläre Zyste
- zystische Hirnmetastasen
- Balkenmangel
- mostly / purely cystic pituitary region masses
- zerebelläre Anomalien
- zystische Hirntumoren
- mikrozystisches Meningeom
- intrakranielle Echinokokkose
- extra axial
- einseitige Kleinhirnaplasie
- unilateral cerebellar hypoplasia
- intrakranielle zystische Läsionen
- Cavum veli interpositi Zyste
- cystic extraaxial mass
- cystic lesion brain
- arachnoid cysts causing proptosis
- Arachnoidalzyste im Kleinhirnbrückenwinkel
- sakrale Arachnoidalzyste
- Arachnoidalzyste, raumfordernd
- parafalcine arachnoid cyst
- Arachnoidalzyste als Ursache eines Hirninfarktes
- arachnoid cyst - parietal
- arachnoid cyst distorting the third ventricle
- eingeblutete Arachnoidalzyste

 Assoziationen und Differentialdiagnosen zu Arachnoidalzyste:
Assoziationen und Differentialdiagnosen zu Arachnoidalzyste:












