Phrenikusparese














Phrenic nerve palsy (also known as phrenic nerve paresis or paralysis) has many causes and can be caused by lesions anywhere along the course of the phrenic nerve, as it travels from the neck, to pierce the diaphragm adjacent to the pericardium.
Epidemiology
No single demographic is affected, as there are numerous causes of a phrenic nerve palsy. The epidemiology will therefore match that of the underlying etiology.
Clinical presentation
Clearly presentation will depend on the underlying cause. In many cases of unilateral (majority of cases) phrenic nerve paralysis, patients are asymptomatic . When presentation is directly attributable to phrenic nerve palsy, then patients typically report dyspnea and orthopnea. Respiratory function tests tend to have a restrictive pattern .
In cases of bilateral phrenic nerve paralysis, symptoms are not surprisingly more pronounced but are particularly exacerbated when recumbent .
Pathology
Etiology
Many cases are idiopathic or thought to be postviral . Common causes include:
- malignancy
- bronchogenic carcinoma
- pulmonary metastases
- mediastinal tumors or neck malignancy
- trauma and iatrogenic
- penetrating injury
- chiropractic manipulation
- postoperative: especially cardiac: up to 10% of cases
- central venous catheters
- direct trauma
- compression by hematoma
- local anesthetic infiltration
- intrascalene brachial plexus nerve blocks
- incidence reduced with ultrasound guidance and use of lower volumes of local anesthetic
- forceps delivery (newborn)
- neuromuscular diseases
- inflammation
- direct compression
- aortic aneurysm
- cervical osteophytes
Radiographic features
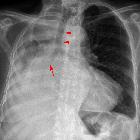
Plain radiograph
In some cases the diagnosis is obvious. However, as diaphragmatic position is not symmetric, an understanding of the normal level of the diaphragms is important (see normal position of diaphragms on chest radiography). If the left hemidiaphragm is higher than the right or the right is higher than the left by more than ~2 centimeters, one of the many causes of diaphragmatic elevation should be sought. This, of course, includes phrenic nerve palsy .
Fluoroscopy
Fluoroscopic examination of the diaphragm ("sniff test") is useful in assessing diaphragmatic function and involves rapid inspiratory effort and observation of the hemidiaphragms.
In normal subjects, both hemidiaphragms descend with inspiration. In cases of phrenic nerve paralysis, the affected side demonstrates paradoxical upward movement .
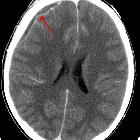
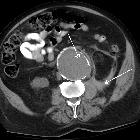
CT
CT has little role in the diagnosis of an elevated hemidiaphragm, as supine position and variable inspiratory effort can significantly alter diaphragmatic height . Despite this, it excels at identifying many of the causes of phrenic nerve palsy and is able to acquire volumetric data from base of skull to upper abdomen.
MRI
MRI is particularly suited to evaluation of Pancoast tumors, and better able to determine tumor extension in such cases.
Conduction and electromyographic studies
Phrenic nerve conduction studies can be carried out with placement of an esophageal electrode to record diaphragmatic contractions and stimulation of the nerve in the neck either with surface stimulation or with a monopolar needle electrode at the level of the cricoid cartilage .
Alternatively, diaphragmatic electromyography may be carried out. The two tests are complementary .
Fluoroscopy may also be employed at the time of conduction studies to confirm diaphragmatic movement.
Treatment and prognosis
In symptomatic unilateral cases, or more often bilateral involvement, diaphragmatic pacing may be used. This can either take the form of distal phrenic nerve stimulation or direct muscular stimulation with implanted electrodes .
Prognosis is influenced by the underlying cause. Nerve function does not usually recover in cases of neoplastic involvement. Like other compressive neuropathies, paralysis is due to compressive lesions, gradual improvement may take place, although this often takes many months or even years .
Differential diagnosis
The differential of a phrenic nerve palsy is essentially that of an elevated hemidiaphragm with common entities to be considered being:
- masses/collections pushing the diaphragm up from below
- hepatic mass
- subphrenic collection
- intra-abdominal fat
- reduced volume of the lung pulling the diaphragm up
- diaphragmatic eventration
In cases of bilateral diaphragmatic paralysis, in addition to bilateral phrenic nerve palsy a number of conditions should be considered :
- high spinal cord injury
- central hypoventilation syndrome (Ondine's curse)
Siehe auch:

 Assoziationen und Differentialdiagnosen zu Phrenikusparese:
Assoziationen und Differentialdiagnosen zu Phrenikusparese: