idiopathic intracranial hypertension
























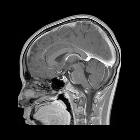
Idiopathic intracranial hypertension (IIH), also known as pseudotumor cerebri, is a syndrome with signs and symptoms of increased intracranial pressure but where a causative mass or hydrocephalus is not identified.
Terminology
The older term benign intracranial hypertension is generally frowned upon due to the fact that some patients with idiopathic intracranial hypertension have a fairly aggressive clinical picture with rapid visual loss.
Interestingly as it has become evident that at least some patients present with IIH due to identifiable venous stenosis, some authors now advocate reverting to the older term pseudotumor cerebri as in these patients the condition is not idiopathic . An alternative approach is to move these patients into a group termed secondary intracranial hypertension .
Epidemiology
By far the most common affected demographic is middle-aged obese females, although the etiological link between being female, overweight and developing idiopathic intracranial hypertension remains to be elucidated. Less commonly idiopathic intracranial hypertension can also be encountered in males, usually older, and less likely to be obese . Idiopathic intracranial hypertension is rare in the pediatric population .
Associations
A variety of conditions are known to be associated with idiopathic intracranial hypertension including:
- endocrine
- adrenal insufficiency
- Cushing disease
- hypoparathyroidism
- hypothyroidism
- excessive thyroxine replacement in children
- drugs
- doxycycline
- chronic renal failure
- systemic lupus erythematosus (SLE)
- hypervitaminosis A (in the pediatric population)
- dural venous sinus stenosis or web: rare but treatable cause of IIH
Clinical presentation
The presentation is usually with headaches, visual problems (transient or gradual visual loss), pulse-synchronous tinnitus, photopsia and eye pain .
Papilledema may not always be present or may be unilateral (including pseudo-Foster Kennedy syndrome), making the clinical diagnosis less than straightforward . Neurological examination is usually normal, with a sixth cranial nerve palsy sometimes encountered.
Additional clinical findings include normal CSF composition with elevated opening pressure. It should be noted that opening pressure varies significantly. One study continuously measuring CSF pressures demonstrated a mean pressure of less than 35 mmHg (48 cm H2O) but with intermittent pressure waves as with amplitudes of 50–80 mmHg (68–109 cm H2O) which lasted 5 to 20 minutes) .
Aberrant arachnoid granulations, also referred to as meningoceles, can result in secondary CSF leak can present as rhinorrhea, otorrhea, intracranial hypotension, and recurrent bacterial meningitis . In such patients it is often only after dural repair that intracranial hypertension becomes evident; presumably, the CSF leak from the meningocele normalized pressure .
Pathology
Idiopathic intracranial hypertension is a poorly understood condition. Various mechanisms have been proposed to explain its pathogenesis, including decreased CSF absorption, increased CSF production, increased intravascular volume, increased intracranial venous pressure and hormonal changes .
Radiographic features
CT/MRI
Imaging of the brain with CT and MRI is essential in patients with suspected idiopathic intracranial hypertension, to exclude elevated CSF pressure due to other causes such as brain tumor, dural sinus thrombosis, hydrocephalus, etc.
In the absence of a cause for intracranial hypertension, imaging features that support the diagnosis of idiopathic intracranial hypertension include :
- optic nerves
- prominent subarachnoid space around the optic nerves (~45%)
- vertical tortuosity of the optic nerves (~40%)
- papilledema
- flattening of the posterior sclera (~80%)
- intraocular protrusion of the optic nerve head
- enhancement of the prelaminar (intraocular) optic nerves (~50%)
- enlarged arachnoid outpouchings
- partially empty sella turcica (~70%) *
- enlarged Meckel cave
- prominent arachnoid pits/aberrant arachnoid granulations/small meningoceles typically within the temporal bone and sphenoid wing
- enlarged CSF space around the oculomotor nerve in the lateral wall of the cavernous sinus
- bilateral venous sinus stenosis
- lateral segments of the transverse sinuses (most important finding)
- no evidence of current or remote thrombosis
- slit-like ventricles (relatively uncommon compared to other findings)
- acquired tonsillar ectopia (mimicking Chiari I malformation)
- increased subcutaneous fat thickness in the scalp and neck
Although bony changes are permanent, the rest are dynamic and may be reversible with treatment .
* It is important to take into account the age and gender of a specific patient in assessing the significance of this finding, as in older patients, especially in males, a partially empty non-enlarged sella is not only common but normal.
Treatment and prognosis
Treatment options include CSF letting, acetazolamide and lumboperitoneal shunts. In patients with progressive visual deterioration, optic nerve fenestration may be required to preserve vision.
Venous sinus stenting has been reported in case series and also being trialed . The treatment is controversial as to whether apparent venous sinus stenosis is the cause or the effect of idiopathic intracranial hypertension . Spontaneous resolution of apparent stenosis is recognized .
History and etymology
Idiopathic intracranial hypertension was first reported in 1893 by Heinrich Quincke, and termed "meningitis serosa". The term "pseudotumor cerebri" was later introduced in 1904, and later still "benign intracranial hypertension" in 1955 (not to be confused with benign intracranial hypotension) .
Differential diagnosis
Other causes of intracranial hypertension and papilledema should be sought. Causes of venous obstruction (e.g. venous sinus thrombosis and venous outflow obstruction in the neck) can very closely mimic the intracranial findings.
Additionally, in patients with prominent cerebellar tonsillar ectopia, the possibility that all findings are in fact due to a Chiari I malformation should be considered, particularly as there is substantial overlap in the demographics and clinical presentation of the two patient groups . It has even been suggested that some cases of symptomatic intracranial hypertension are secondary to a Chiari I malformation . Importantly, however, every attempt should be made to distinguish between the two entities as treatment is different and symptom relief for patients with idiopathic intracranial hypotension with posterior fossa decompression is insignificant .
Siehe auch:
und weiter:

 Assoziationen und Differentialdiagnosen zu Idiopathische intrakranielle Hypertension:
Assoziationen und Differentialdiagnosen zu Idiopathische intrakranielle Hypertension:

