Langerhans cell histiocytosis (skeletal manifestations)






































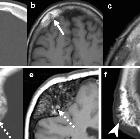
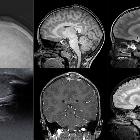
The skeleton is the most commonly involved organ system in Langerhans cell histiocytosis (LCH) and is by far the most common location for single-lesion LCH, often referred to as eosinophilic granuloma (EG) (the terms are used interchangeably in this article). For a general discussion of this disease please refer to the article on Langerhans cell histiocytosis (LCH).
Epidemiology
The skeletal system is the most common site of Langerhans cell histiocytosis involvement, and in 60-80% of cases is the only organ system involved. It primarily occurs in older children and young adults, with a male to female ratio of 2:1.
Clinical presentation
The lesions may be asymptomatic and discovered as an incidental radiographic finding.
When symptomatic, patients complain of pain, swelling and tenderness around the lesion. Systemic symptoms may also be present, including general malaise and, on occasion, fever with leukocytosis.
Pathology
There is proliferation of Langerhans cells with an abundance of eosinophils, lymphocytes and neutrophils. These cells produce prostaglandins which result in medullary bone resorption: this is what causes the symptoms.
Location/distribution
Patients may have one or, less commonly, many lesions. The most common locations are the skull and long bones :
- skull: ~50%
- pelvis: 23%
- femur: 17%
- ribs: 8% (most common in adults)
- humerus: 7%
- mandible: 7%
- spine
Radiographic features
Plain radiographs
Skull
- solitary or multiple punched out lytic lesions without sclerotic rim
- double contour or beveled edge appearance may be seen due to asymmetrical involvement of the inner and outer tables (hole within a hole) sign
- button sequestrum representing residual bone
- geographic skull
Mandible
- irregular radiolucent areas mostly involving superficial alveolar bone
- floating tooth: loss of lamina dura
Spine
- vertebra plana: most common cause of vertebra plana in children; more often in thoracic spine
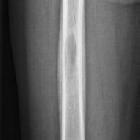
Long bones
- depends on phase of disease which is imaged
- permeative and aggressive appearing lesion
- mainly involves diaphysis or metadiaphysis and respects growth plates
- endosteal scalloping, periosteal reaction (in healing phase it can appear as solid benign periosteal reaction), cortical thinning, intracortical tunneling, and associated soft tissue mass
Ultrasound
Skull
- seen as a solid mass lesion
- minimal vascularity
- originating from the diploic surface, extending through to the outer table
- local subperiosteal spread
CT
Similar to plain film findings with better demonstration of cortical erosion and soft tissue involvement. Excellent for biopsy and surgical planning.
MRI
Signal characteristics include:
- T1: typically hypointense to isointense
- T2: hyperintense
- STIR: hyperintense
- T1 C+ (Gd): often shows diffuse contrast enhancement
Nuclear medicine
There is a variable appearance on bone scintigraphy, with lesions showing an increased or decreased tracer uptake depending on the histological picture. Nonetheless, bone scans are helpful in other asymptomatic lesions.
Treatment and prognosis
Prognosis is excellent when disease is confined to the skeleton, especially if it is a solitary lesion, with the majority of such lesions spontaneously resolving by fibrosis within 1-2 years. However, where symptoms persist, other treatment options may be considered:
- excision and curettage
- steroid therapy: intralesional injection
- chemotherapy
- radiofrequency ablation
- radiotherapy for spinal lesion
History and etymology
The term eosinophilic granuloma was coined by Lichtenstein and Jaffe in 1940.
Differential diagnosis
General imaging differential considerations include:
- osteomyelitis
- round blue cell tumors
- metastases
- primary bone tumors
- lymphoma
- leukemia
Siehe auch:
- Osteolysen der Kalotte
- Osteomyelitis
- Periostreaktion
- Vertebra plana
- Histiozytose X
- button sequestrum
- eosinophiles Granulom des Schädels
- Eosinophiles Granulom der Wirbelsäule
- Hand-Schüller-Christian-Syndrom
- geographic skull
- Langerhans-Zell-Histiozytose der Orbita
- Langerhans-Zell-Histiozytose der Wirbelsäule
- round blue cell tumours
und weiter:
- Langerhanszell-Histiozytose der Lunge
- Platyspondylie
- Tumoren der Hypophysenregion
- einfache (juvenile) Knochenzyste
- solitäre lytische Läsion des Schädels
- moth-eaten appearance in bone
- Aseptische Wirbelkörpernekrose
- verdickter Hypophysenstiel
- vegetable and plant inspired signs
- Sarkoidose ossäre Manifestationen
- epiphysäre Knochentumoren
- retikuläres Muster
- vertebra plana (mnemonic)
- osseous lesions preferentially involving the epiphysis
- diaphyseal lesions (mnemonic)
- PLCH
- lytic bone lesion (mnemonic)
- musculoskeletal manifestations of sarcoidosis
- permeative process in bone (mnemonic)
- bony sequestrum (mnemonic)
- multiple lytic bone lesions (mnemonic)
- lytic rib lesion (mnemonic)
- Sklerosierung der Klavikula
- upper lobe pulmonary fibrosis (mnemonic)
- Sequester
- posterior vertebral body lesions (mnemonic)
- Knochenläsionen der Diaphyse
- Knochenläsionen mit Sequester
- Tumoren der Wirbelsäule
- Osteolyse der Tibia
- eosinophiles Granulom Femur
- pelvic eosinophilic granuloma
- langerhans cell histiocytosis with osseous and pulmonary involvement
- solitary eosinophilic granuloma of the radius
- eosinophilic granuloma of the sternum
- Eosinophiles Granulom der HWS
- Metastasen in der Hypophyse

 Assoziationen und Differentialdiagnosen zu skeletale Manifestationen der Langerhanszell-Histiozytose:
Assoziationen und Differentialdiagnosen zu skeletale Manifestationen der Langerhanszell-Histiozytose: