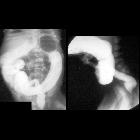
Mekoniumileus







 nicht verwechseln mit: Mekoniumpfropf-Syndrom
nicht verwechseln mit: Mekoniumpfropf-SyndromMeconium ileus refers to a neonatal bowel obstruction of the distal ileum due to abnormally thick and impacted meconium. Unlike in the meconium plug syndrome, the meconium is abnormal in consistency.
Epidemiology
Meconium ileus is more common in white populations and affects both sexes almost equally.
Pathology
Meconium found in the intestine of a neonate consists of succus entericus (bile salts, bile acids, and debris from the intestinal mucosa) and is normally evacuated within 6 hours of birth (or earlier).
Meconium ileus occurs when meconium becomes inspissated and obstructs the distal ileum. It is usually a manifestation of cystic fibrosis. Approximately 20% of infants with cystic fibrosis present with meconium ileus at birth.
Although it is usually understood as synonymous with cystic fibrosis until proven otherwise, it may also be seen with pancreatic atresia or stenosis of the pancreatic duct.
Only rarely does it occur without cystic fibrosis or pancreatic abnormality, and is thought to be related to gut immaturity (more favorable outcome).
Radiographic features
Plain radiograph
Non-specific and may show dilated bowel loops proximal to the impaction. Classically, there is a paucity or absence of air-fluid levels and a "bubbly" appearance of the distended intestinal loops on radiographs. Occasionally, has a mottled appearance on radiographs during the first 2 days of life.
Fluoroscopy
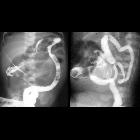
Contrast enema will show a microcolon involving the entire large bowel and may show impacted meconium pellets filling defects, particularly in the right colon or in the distal ileum.
Ultrasound
Prenatal ultrasound findings associated with meconium ileus include
- echogenic bowel, which can be dilated and thick walled
- polyhydramnios
- fetal ascites
- peritoneal wall calcifications
- intra-abdominal cysts
Treatment and prognosis
Water-soluble contrast enema usually clears the impacted meconium, with a success rate of over 60%.
Complications
- ileal atresia or stenosis
- ileal perforation resulting in meconium peritonitis
- volvulus with or without pseudocyst formation
Differential diagnosis
General imaging differential considerations include
- total colonic Hirschsprung disease
- meconium plug syndrome
Siehe auch:
und weiter:

 Assoziationen und Differentialdiagnosen zu Mekoniumileus:
Assoziationen und Differentialdiagnosen zu Mekoniumileus: