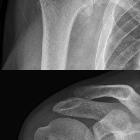
Neuropathic arthropathy















































Charcot joint, also known as a neuropathic joint or Charcot (neuro/osteo)arthropathy, refers to a progressive degenerative/destructive joint disorder in patients with abnormal pain sensation and proprioception.
Epidemiology
In modern Western societies by far the most common cause of Charcot joints is diabetes mellitus, and therefore, the demographics of patients match those of older diabetics. Prevalence differs depending on the severity of diabetes mellitus :
- ~0.1% in general diabetic population
- ~15% in high-risk diabetic population
- ~30% in patients with peripheral neuropathy
Clinical presentation
Patients present insidiously or are identified incidentally, or as a result of investigation for deformities. Unlike septic arthritis, Charcot joints although swollen are normal temperature without elevated inflammatory markers. Importantly, they are painless.
Pathology
The pathogenesis of a Charcot joint is thought to be an inflammatory response from a minor injury that results in osteolysis. In the setting of peripheral neuropathy, both the initial insult and inflammatory response is not well appreciated, allowing ongoing inflammation and injury .
Charcot joints are typically unilateral but are bilateral in ~20% (range 5.9-39.3%) of cases . There are two patterns of Charcot joint: atrophic and hypertrophic.
Atrophic form
- most common form
- occurs earlier
- has an acute progression
- characterized by reabsorption of the ends of the affected bone
- joint destruction with resorption of fragments
- an absence of osteosclerosis and osteophytes
- mainly occurs in non-weight bearing joints of the upper limb
Hypertrophic form
- only sensory nerves affected
- slow progression
- joint destruction with periarticular debris/bone fragmentation
- initially widened then narrowed joint space
- presence of osteosclerosis and osteophytes
- absence of osteoporosis (unless joint is infected)
Etiology/Location
Sensorimotor and autonomic neuropathies of various etiologies are the primary predisposing factor. The most common etiology varies by the involved joint :
- diabetes mellitus (most common cause overall and in the foot and ankle; most commonly affects the foot and ankle)
- syringomyelia (most common cause in the upper extremity and shoulder)
- neurosyphilis/tabes dorsalis (more common in the past; most commonly affects the knee)
- traumatic spinal cord injury (most common cause in the spine)
- alcoholism
- tumors compressing or involve the spinal cord or peripheral nerves
- amyloidosis
- pernicious anemia
- poliomyelitis
- leprosy
- multiple sclerosis
- steroid use (intraarticular or systemic)
- spina bifida/myelomeningocele
- congenital insensitivity to pain
- Charcot-Marie-Tooth disease
- familial dysautonomia (Riley-Day syndrome)
Less established causes:
Some of these can be recalled with the "S" mnemonic.
Radiographic features
Plain radiograph and CT
Charcot arthropathy appears as a destructive and disorganizing process centered in the joint and affecting surrounding bones, which may mimic severe osteoarthritis or septic arthritis . Manifestations depend on stage :
- development/fragmentation/dissolution: subchondral osteopenia is the earliest finding , followed by bony fragmentation (with formation of debris seen as intraarticular loose bodies) and joint malalignment (subluxation or dislocation due to ligamentous laxity)
- coalescence: bony consolidation begins with subchondral sclerosis, periosteal bone formation, and fusion of the larger fragments and absorption of the smaller fragments
- reconstruction/reconstitution: remodeling occurs with rounding of fragments and ankylosis, making deformity permanent
General characteristics may be recalled with the six Ds mnemonic.
MRI
MRI plays an important role in diagnosing complications, assessing the extent of the disease, and presence of osteomyelitis.
- T1:
- involved joints appear diffusely swollen, showing decreased signal intensity
- fat planes adjacent to ulcerated skin show decreased signal intensity
- if superinfected with a gas-producing organism, there will be a loss of signal intensity.
- T1 C+ (Gd): inflammatory areas show enhancement, with central non-enhancing necrotic areas
- STIR:
- early infection: increased signal intensity due to marrow edema
- later stages: loss of demarcation of cortical outline and cortical destruction
Differential diagnosis
Imaging differential considerations include:
- advanced osteomyelitis: can co-exist (especially in the foot)
- tuberculous spondylitis or Pott's disease (in the spine)
- chondrosarcoma (shoulder): chondroid matrix instead of bony debris
- inflammatory osteoarthritis/arthritis: early stages can resemble Charcot joint
History and etymology
The French pathologist and neurologist Jean-Martin Charcot (1825-1893), the "father of neurology" was the first person to give a detailed description of the neuropathic aspect of this condition in 1868 in a patient suffering syphilis .
Practical points
Useful MRI features that support superimposed osteomyelitis on a Charcot joint include :
- sinus tract
- diffuse marrow signal abnormality
- replacement of soft tissue fat
- thick rim enhancement
- joint erosion
- ghost sign
Siehe auch:
- Osteomyelitis
- Chondrosarkom
- Gicht
- Arthrose
- Gichtfuß
- tuberkulöse Spondylitis
- Müller-Weiss-Syndrom
- Madurafuß
- Lisfranc-Gelenklinie
- bone leprosy of the feet
- Abszess Fuß
und weiter:
- Frakturen mit Eigennamen
- Diabetes mellitus
- Neurolues
- Spondylodiscitis
- Lisfranc Luxationsfraktur
- Discitis
- Milwaukee-Schulter
- differential diagnosis for metatarsal region pain
- Talus verticalis
- Myzetom
- mycetoma foot
- very bizarre generalised lesions (mnemonic)
- Osteitis Diabetes
- charcot joint features (mnemonic)
- diabetic osteomyelitis
- diabetic callus
- Klavus
- charcot joint - spine
- a neuropathic hip joint with loose-body formation
- features of a Charcot joint (mnemonic)

 Assoziationen und Differentialdiagnosen zu diabetisches Fußsyndrom:
Assoziationen und Differentialdiagnosen zu diabetisches Fußsyndrom: