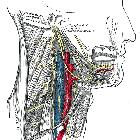
vertebral artery



























The vertebral arteries (VA) are paired arteries, each arising from the respective subclavian artery and ascending in the neck to supply the posterior fossa and occipital lobes, as well as provide segmental vertebral and spinal column blood supply.
Summary
- origin: branches of the 1st part of the subclavian artery
- course: ascends posterior to the internal carotid artery in the transverse foramina of the cervical vertebrae
- branches
- numerous small branches
- radicular/spinal branches
- posterior inferior cerebellar artery (PICA)
- termination: combines with the contralateral vertebral artery to form the basilar artery
- key relationships: posterior to the internal carotid artery; ascends anterior to the roots of the hypoglossal nerve (CN XII)
Gross anatomy
Origin
The origin of the vertebral arteries is usually from the posterior superior part of the subclavian arteries bilaterally, although the origin can be variable:
- brachiocephalic artery (on the right)
- aortic arch: 6% of cases, most on the left
The VA is normally 3-5 mm in diameter and the ostium is the most common site of stenosis.
When the origin is from the arch, then it is common for the artery to enter the foramen transversarium at a level higher than normal (C5 instead of C6).
Segments
The vertebral artery is typically divided into 4 segments:
- V1: pre-foraminal segment
- origin to the transverse foramen of C6
- V2: foraminal segment
- from the transverse foramen of C6 to the transverse foramen of C2
- V3: atlantic, extradural or extraspinal segment
- starts from C2, where the artery loops and turns lateral to ascend into the transverse foramen
- continues through C1 to pierce the dura
- V4: intradural or intracranial segment
- from the dura at the lateral edge of the posterior atlanto-occipital membrane to their confluence on the medulla to form the basilar artery
Course
V1 (pre-foraminal)
Also known as the extraosseous segment, V1 arises from the first part of the subclavian artery. It angles posteriorly between longus colli medially and scalenus anterior laterally, through the colliscalene triangle, and behind the common carotid artery to enter the transverse foramen of C6.
Relations:
- anteriorly: common carotid artery, vertebral vein, thoracic duct (left VA), and lymphatic duct (right VA)
- posteriorly: ventral rami of spinal nerves C7 and C8, transverse process of C7, inferior cervical ganglion
- anteromedially: inferior thyroid artery, middle cervical ganglion
V2 (foraminal)
V2 ascends through the transverse foramina of the cervical vertebrae, normally C6-C3. Here it is accompanied by the vertebral veins and the sympathetic nerves. It then turns superolaterally through the inverted L-shaped transverse foramen of C2.
V3 (atlantic, extradural or extraspinal)
V3 emerges from the transverse process of C2 (axis) and sweeps laterally to pass through the transverse foramen of C1 (atlas). From here it passes around the posterior border of the lateral mass of C1 and below the inferior border of the posterior atlanto-occipital membrane lateral to the cervico-medullary junction. Passing superomedially it pierces the spinal dura and arachnoid to continue as V4. This tortuosity provides length and freedom for the vessel to stretch, straighten and bend during rotation of the head, which occurs at the atlanto-axial joints.
V4 (intradural or intracranial)
V4 ascends anterior to the roots of the hypoglossal nerve (CN XII) and joins its contralateral counterpart at the lower border of the pons to form the basilar artery.
Branches
Numerous muscular branches are given off as the artery ascends, with relatively large ones passing posteriorly from V3 to supply the occipital triangle. They can anastomose with occipital branches of the ECA.
Spinal branches, pass into the spinal canal via the intervertebral foramina and contribute to supply not only of the vertebral bodies and extradural content of the canal but also of the dura and spinal cord, reinforcing the anterior and posterior spinal arteries.
The posterior inferior cerebellar artery (PICA) is the largest branch of the vertebral artery and is one of three main arteries supplying the cerebellum.
Other branches include:
- V1: segmental cervical muscular and spinal branches
- V2: anterior meningeal artery, muscular and spinal branches
- V3: posterior meningeal artery
- V4: anterior and posterior spinal arteries (ASA and PSA), perforating branches to medulla, posterior inferior cerebellar artery
Supply
- ASA: upper cervical spinal cord, inferior medulla
- PSA: dorsal spinal cord to conus medullaris
- PICA: lateral medulla, tonsil, inferior vermis/cerebellum, choroid plexus of 4 ventricle
- penetrating branches: portion of the medulla, olives, inferior cerebellar peduncle
Variant anatomy
- asymmetry due to vertebral arterial hypoplasia, absence or termination into PICA of one of the vertebral arteries is very common
- left dominant ~45% (range 42-50%)
- right dominant ~30% (range 25-32%)
- co-dominant ~25% (range 25-26%)
- complete or partial vertebral artery duplication
- vertebral artery fenestration (predisposes to aneurysms)
- variable origin
- single left aberrant origin (86%), single right aberrant (12%), bilateral aberrant origin (3%)
- aortic arch origin of left vertebral artery: incidence ~5% (range 3.1-8.3%)
- second (not first) branch of subclavian artery
- external carotid artery (rare) - see case 14
- common carotid artery (rare) - see case 15
- internal carotid artery (rare)
- ostium may have variable orientation
- cranial ~47%
- posterior ~45%
- caudal ~5%
- anterior ~3%
Ultrasound assessment
- velocities can have a wide range amongst individuals ranging from 20-60 cm/s
- luminal diameter may increase slightly with age .
- due to a pronounced decrease in end-diastolic flow velocity, the resistance index can decrease during aging.
Related pathology
- vertebral artery thrombosis
- vertebral artery dissection
- rotational occlusion of the vertebral artery (Bowhunter syndrome)
Siehe auch:
- Normvarianten der Arteria vertebralis
- Arteria carotis interna
- Dissektion Arteria vertebralis
- Arteria basilaris
- Abgang der linken Arteria vertebralis aus der Aorta
- Musculus scalenus anterior
- Foramen transversarium
- Nervus hypoglossus
- Arteria vertebralis Segmente
- Thrombose Arteria vertebralis
- intravertebraler Verlauf der Arteria vertebralis
- hinteres Stromgebiet
und weiter:
- intrakranielle Verkalkungen
- Foramen arcuale
- fenestrierte Arteria basilaris
- subclavian artery branches (mnemonic)
- Circulus Willisi
- Dura mater
- Brain stone
- Arteria spinalis anterior
- Arteria trigemina
- posterior cerebral circulation
- arterielle Versorgungsgebiete des Gehirns
- Aortenbogen
- labyrinthine artery
- persistent hypoglossal artery
- Spasmus hemifacialis
- persistent proatalantal intersegmental artery
- Varadi-Papp-Syndrom
- Duplikation der Arteria vertebralis
- hyperdense artery sign - vertebral artery
- intrakranielle Arteriosklerose
- intrakranielle Arterien
- Arterien von Kopf und Hals
- Very Tired Individuals Sip Strong Coffee Served Daily

 Assoziationen und Differentialdiagnosen zu Arteria vertebralis:
Assoziationen und Differentialdiagnosen zu Arteria vertebralis: