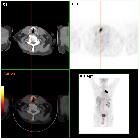
vocal cord paralysis










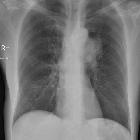























Vocal cord paralysis/paresis (VCP), also known as vocal fold paralysis/paresis, refers to the impaired mobility of the true vocal cord or fold due to neurologic dysfunction.
Clinical presentation
Unilateral vocal cord paralysis usually presents with dysphonia (hoarseness), characterized as a breathy, weak voice due to air leaking through the glottic gap as one vocal cord is unable to adduct fully. Patients may also complain of dysphagia or choking as glottic incompetence increases the risk of aspiration.
Bilateral vocal cord paralysis may present as dyspnea if the paralyzed cords rest close to the midline, reducing the glottic area available for air movement.
The diagnosis may also be made incidentally on laryngoscopy or imaging as up to one-third of patients with impaired vocal cord impairment are asymptomatic .
Pathology
Neurologic dysfunction resulting in vocal cord paralysis most common localizes to the recurrent laryngeal nerve, but can also be due to upstream lesions affecting the vagus nerve (from which the recurrent laryngeal nerve branches off) or the brain. Injury to the recurrent laryngeal nerve affects motor function of most of the intrinsic laryngeal muscles (posterior cricoarytenoid, lateral cricoarytenoid, transverse arytenoid, oblique arytenoid, and thyroarytenoid).
In comparison, injury to the superior laryngeal nerve, which supplies only the cricothyroid muscle, causes subtle changes in voice and is less clinically significant.
Unilateral involvement is much more common than bilateral involvement . The left side is most commonly affected, likely because the longer course of the left recurrent laryngeal nerve presents greater opportunity for injury.
Etiology
- superior thoracic masses, e.g. lung cancer (most common ), aortic pathologies (e.g. thoracic aortic aneurysm), thyroid cancer, laryngeal cancer
- masses affecting the vagus nerve, e.g. jugular foramen masses, carotid body tumors
- surgical iatrogenic injury, especially post thyroidectomy
- idiopathic
- blunt and penetrating trauma in the head and neck, and thorax
- congenital anomalies, e.g. meningomyelocele, Chiari malformation, hydrocephalus
Radiographic features
The imaging features of vocal cord paralysis include the following:
- enlarged pyriform sinus
- medialization and thickening of the aryepiglottic fold
- enlarged laryngeal ventricle (sail sign)
- atrophy of the thyroarytenoid muscle, which makes up the bulk of the true cord
- anteromedial deviation of the arytenoid cartilage
- abducted vocal cord during breath-hold imaging with compensatory medial bowing of the contralateral cord
- atrophy of the posterior cricoarytenoid muscle
Laryngeal ultrasonography allows dynamic, real-time assessment of vocal fold adduction and abduction, and has demonstrated high fidelity with the diagnostic gold standard, flexible endoscopy . The most commonly utilized sonographic window is obtained by placing the (linear or curvilinear) transducer on the midline neck, seeking a transverse window through the thyroid cartilage. Supine patient positioning with slight neck extension during the exam is optimal.
- sonographic landmarks are the true vocal folds, false vocal folds, and arytenoid cartilages
- the true vocal folds are hyperechoic and the more superficial of the structures
- the presence and symmetry of vocal fold motion is assessed through eliciting quiet inspiration, an apneic pause, and phonation
- unilateral absence of true/false folds and arytenoid motion, typically accompanied by compensation of the contralateral structures, is highly indicative of unilateral vocal cord paralysis
Practical points
When vocal cord paralysis has been diagnosed, a cause should be actively sought along the course of the recurrent laryngeal nerve from origin in the brainstem, through the neck, and should always include the superior mediastinum.
Siehe auch:
- Larynx
- Nervus laryngeus recurrens
- Plica vocalis
- Larynxmuskulatur
- Heiserkeit
- Ortner-Syndrom 1 - cardiovokales Syndrom
und weiter:

 Assoziationen und Differentialdiagnosen zu Rekurrensparese:
Assoziationen und Differentialdiagnosen zu Rekurrensparese: