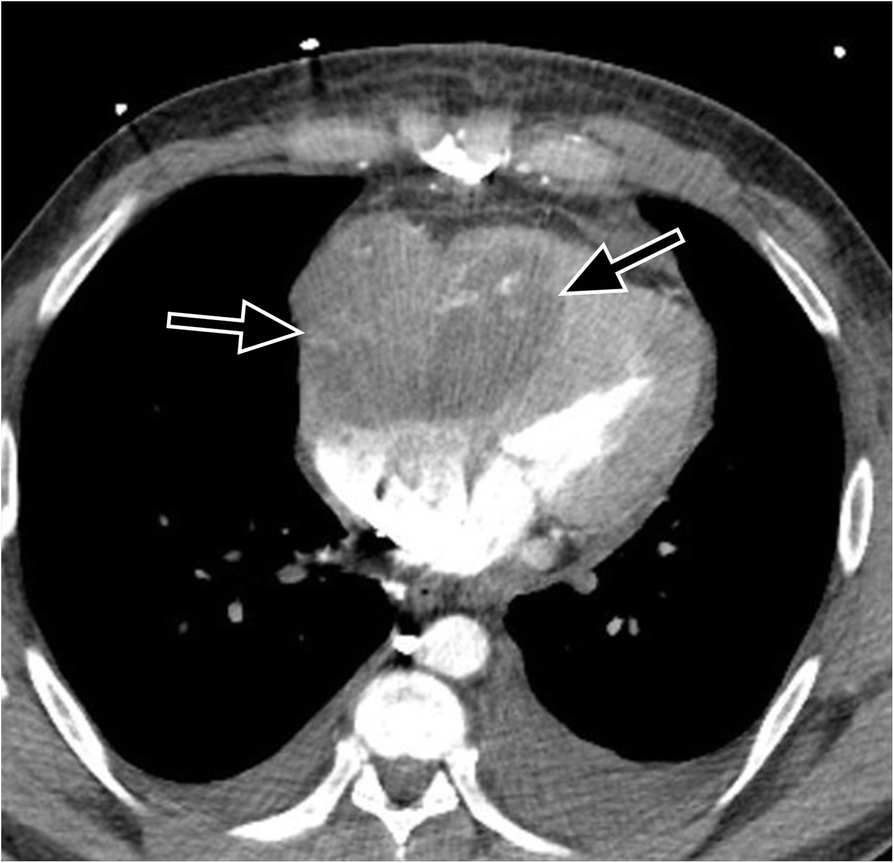
atrial myxoma

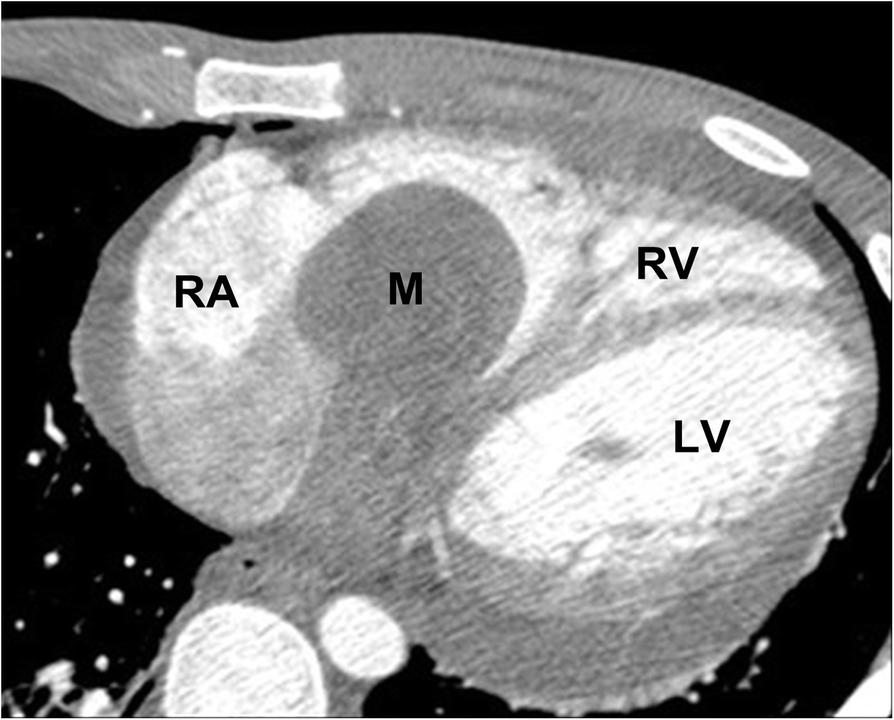
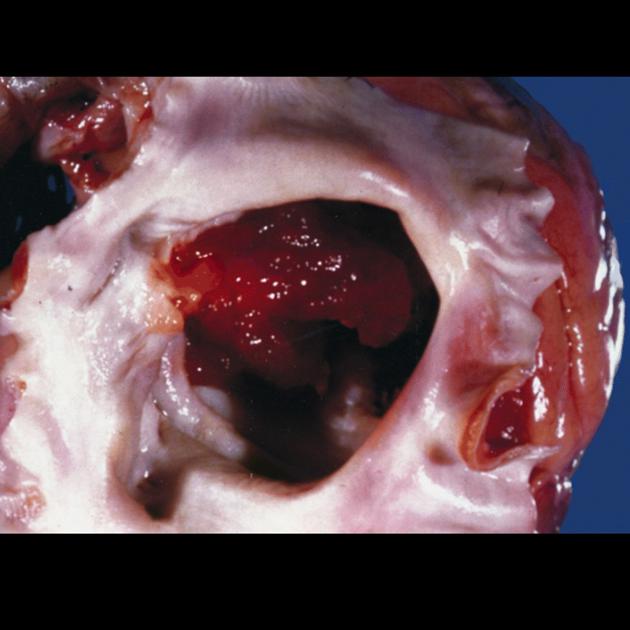
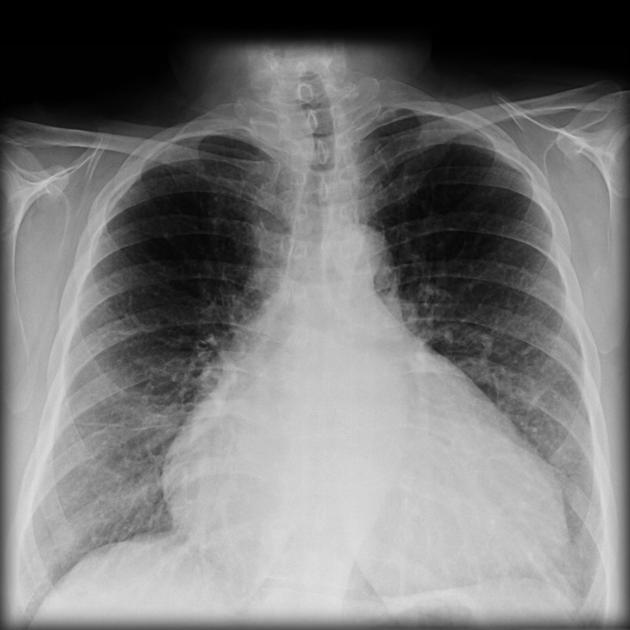
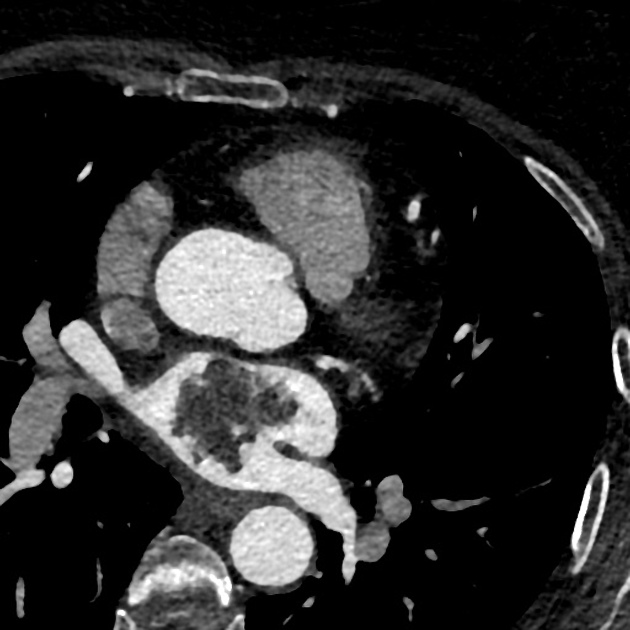
Cardiac myxomas, although uncommon are one of the commonest primary cardiac tumors and account for ~50% primary benign cardiac tumors.
Epidemiology
Cardiac myxomas are the most common primary cardiac tumor in adults (~50%) but are relatively infrequent in childhood, where cardiac rhabdomyomas are more frequent . The incidence of cardiac myxomas is approximately 0.5 per million population per year . There is a broad range in the age of presentation (11-82 years), with most patients presenting in adulthood (mean ~50 years of age) . There is a recognized female predilection .
Clinical presentation
Approximately 20% of patients are asymptomatic, with myxomas being found incidentally on imaging of the heart. Presumably, as the amount of imaging increases, so will this figure.
Clinical features are variable and depend on the location and other associated pathology, e.g. valve destruction. However, a triad of symptoms is recognized :
- left sided: dyspnea, orthopnea, pulmonary edema
- right sided: symptoms of right heart failure
- distribution will depend on the location of the tumor
- most are left sided, and, therefore, most are systemic (brain or extremities)
- weight loss, fatigue, weakness
- may resemble infective endocarditis (fever, arthralgia, lethargy)
In ~20% of patients, arrhythmias may be identified .
On auscultation, a cardiac murmur is usually present. A characteristic finding in patients with pedunculated and prolapsing myxoma is the so-called "tumor plop" .
Pathology
Controversy exists in regards to the exact nature of these masses, but in general, they are considered benign neoplasms. Some authors believe that they represent organized thrombus.
Morphologically they are often hemorrhagic and are of variable firmness. They can be sessile or pedunculated (commoner) and of variable size (1-10 cm). They most frequently arise in the left atrium, attached to the interatrial septum in the region of the fossa ovale.
Location
Patients with atrial myxomas can be divided into two groups: typical (vast majority) and atypical :
- typical: solitary with ~75% located in the left atrium
- atypical: earlier presentation; multiple tumors are common and are more frequently located in the right heart or left ventricle
Overall distribution :
- atria (95%)
- left (75%)
- right (20%)
- ventricles (5%)
Associations
An uncommon but well-described association with multiple endocrine neoplasia syndromes has been described, and is known as Carney complex .
Radiographic features
Plain radiograph
Chest radiographs can be normal . Abnormalities, if present, are non-specific and include:
- cardiomegaly: left atrial enlargement
- intracardiac tumoral calcification
- evidence of mitral valve obstruction
- evidence of elevated left atrial pressure, e.g. pulmonary edema
Ultrasound
Echocardiography is usually the initial modality used for identification and evaluation of cardiac myxomas. They appear as hyperechogenic lesions with a well-defined stalk. Moreover, echocardiography can be useful to assess the mobility of the tumor, as it often protrudes through valve flaps.
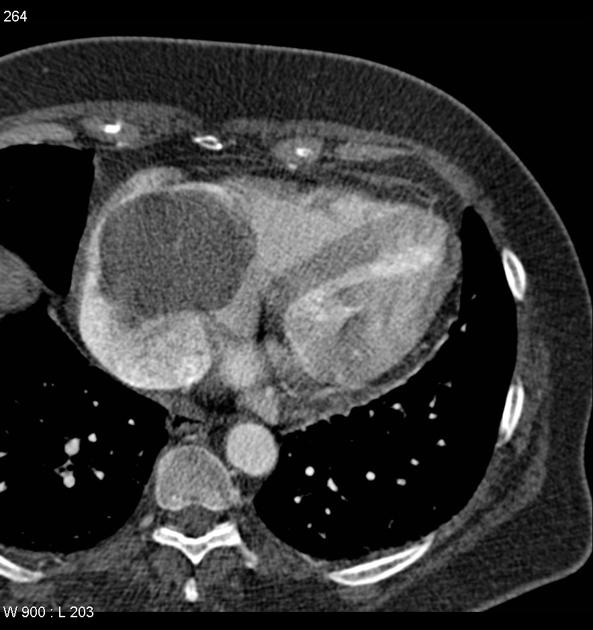
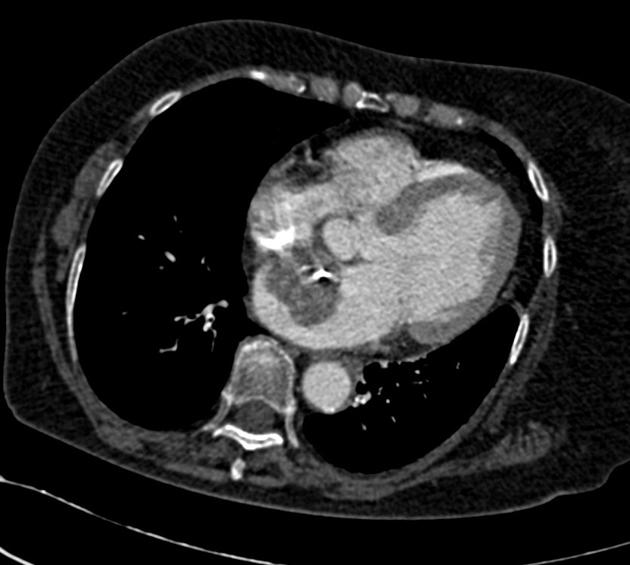
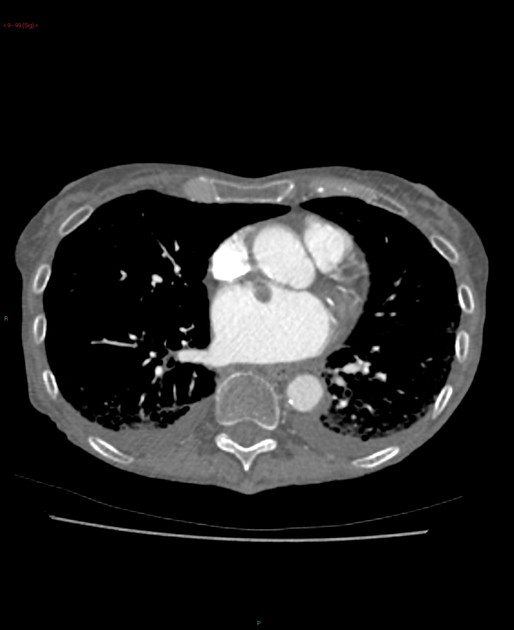
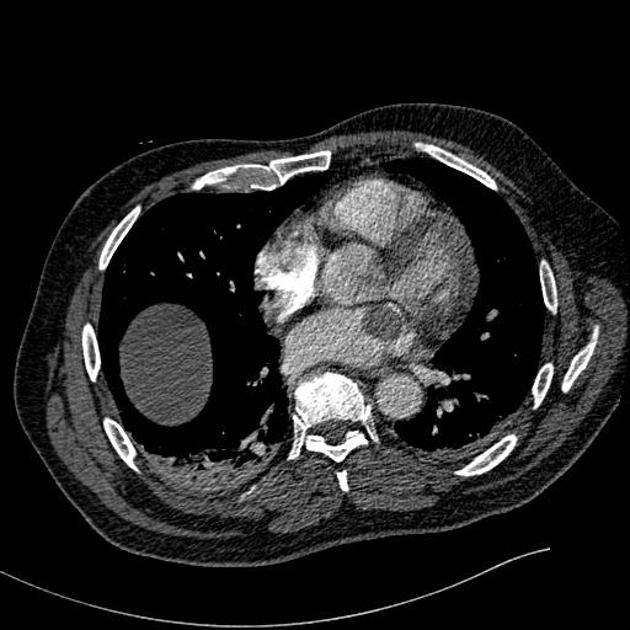
CT
Myxomas, as is the case with other cardiac tumors, appear as intracardiac masses, most often in the left atrium and attached to the interatrial septum. They are usually heterogeneously low attenuating (approximately two-thirds of cases ). Due to repeated episodes of hemorrhage, dystrophic calcification is common .
If the mass is pedunculated, the motion within the heart can be demonstrated, including prolapse through the mitral valve.
MRI
MRI appearances are heterogeneous, reflecting the non-uniformity of these masses. They are typically spherical or ovoid masses which may be sessile or pedunculated .
- T1: tend to be low to intermediate signal, but areas of hemorrhage may be high
- T2: can be variable due to heterogeneity in tumor components; e.g. calcific components > low signal; myxomatous components > high signal
- GE (gradient echo): may show blooming of calcific components
- T1 C+ (Gd): shows enhancement (important discriminator from a thrombus)
Treatment and prognosis
Complete resection in typical cases is usually curative with recurrence rates (either locally or elsewhere in the heart) reported in 0-5% of cases. In atypical cases or those with Carney complex, the rate is much higher (12-22%) .
Complications
- cardiac arrhythmia(s)
- embolic complications, e.g. stroke, hemorrhage from neoplastic intracranial aneurysm
Differential diagnosis
On imaging consider
Siehe auch:
- intrakardiale Thromben
- Lipomatöse Hypertrophie des interatrialen Septums
- Tumoren des Herzens
- Vorhofthrombus
- Myxom des linken Vorhofs
- verkäsende Kalzifikation der Mitralklappe
- primäre kardiale Tumoren
und weiter:

 Assoziationen und Differentialdiagnosen zu Vorhofmyxom:
Assoziationen und Differentialdiagnosen zu Vorhofmyxom: