Behcet syndrome


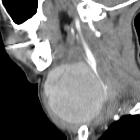













Behçet disease is a multisystemic and chronic inflammatory vasculitis of unknown etiology.
Epidemiology
The mean age at which Behçet disease occurs is 20-30 years. The disease is most prevalent in the Mediterranean region, Middle East and East Asia. The highest incidence has been reported in Turkey. Males are affected 2-5 times more often than females.
Clinical presentation
The classic clinical triad of Behçet disease consists of:
Additional clinical manifestations include skin, joints, gastrointestinal tract, genitourinary tract, central nervous system, cardiovascular system, and lung involvement. Vascular complications develop in ~30% (20-40%) of patients with Behçet disease.
Pathology
The underlying pathologic process in Behçet disease is vasculitis, and perivascular inflammatory infiltrates affecting vessels of differing sizes in various organs.
Associations
Distribution
Primarily involves four main systems:
- cardiovascular manifestations of Behçet disease
- affects 5-30% of cases
- thickening of the aorta and superior vena cava (vasculitis)
- inflammation of the veins leads to thrombosis while arterial involvement includes arterial narrowing and aneurysmal dilatation
- pericarditis is the most common cardiac manifestation occurring in 39% of cases
- thoracic manifestations of Behçet disease
- affects 1-8% of cases
- pulmonary arterial aneurysm: fusiform to saccular, commonly multiple and bilateral, located in the lower lobe or main pulmonary arteries (most common pulmonary manifestation of Behçet disease)
- subpleural alveolar infiltrates, and wedge-shaped or rounded areas of increased density, which represent focal vasculitis and thrombosis resulting in infarction, hemorrhage, and focal atelectasis
- gastrointestinal manifestations of Behçet disease: affects 5-60% of cases
- CNS manifestations of Behçet disease: affects 10-50% of cases
- musculoskeletal manifestations of Behçet disease: >50% develop articular disorders or arthralgia
Treatment and prognosis
The disease may recur, progress, or resolve (either spontaneously, within a few weeks to several months, or with corticosteroid therapy).
History and etymology
It is named after Hulusi Behçet (1889-1948), Turkish dermatologist.
Differential diagnosis
On imaging consider:
Siehe auch:
und weiter:
- Aneurysma spurium
- Vaskulitis
- Ileitis terminalis
- Aortitis
- Sakroiliitis
- Nierenarterienaneurysma
- posttraumatisches Aneurysma spurium
- bilateral middle cerebellar peduncle lesions
- pulmonale Vaskulitis
- Erythema nodosum
- Aneurysma der Arteria pulmonalis
- traumatic pseudoaneurysm
- stroke in children and young adults
- Aneurysma Arteria carotis
- differential diagnosis of intramuscular high STIR signal on MRI
- Rasmussen-Aneurysma
- Muskelödem
- carotid artery pseudoaneurysm and multiple pulmonary artery aneurysms due to Behcet's disease
- Großgefäßvaskulitis
- Pseudoaneurysma der Arteria carotis
- Aneurysma spurium der Pulmonalarterien
- Vaskulitis im Gastrointestinaltrakt

 Assoziationen und Differentialdiagnosen zu Morbus Behçet:
Assoziationen und Differentialdiagnosen zu Morbus Behçet:
