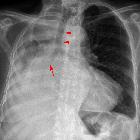
Dermatomyositis

















Dermatomyositis is an autoimmune inflammatory myositis, which like its closely-related condition polymyositis, carries an increased risk of malignancy.
Epidemiology
There is a recognized female predilection. It has a bimodal age of presentation depending on the variant:
- juvenile dermatomyositis (JDM): affects children and tends to be more severe
- adult dermatomyositis (ADM): typically affects adults around the age of 50
Associations
- interstitial lung disease : typically gives a patchy and subpleural consolidation with parenchymal bands
- internal malignancy : can occur as part of a paraneoplastic syndrome (e.g. lung cancer)
Clinical presentation
The classic presentation is that of a symmetrical proximal myopathy with associated dermatological changes which includes a dusky-red rash over the face, arms, hands, legs and other features (e.g. Gottron papules). Dysphagia, myalgia, fever and weight loss are other features .
Complications
Malignancy
There is a sixfold increased risk of malignancy in dermatomyositis (cf. twofold in polymyositis) . Multiple risk factors for the development of malignancy have been identified :
- >60 years old
- male
- dysphagia
- necrosis of the skin
- cutaneous vasculitis
- accelerated onset of disease
- increased creatine kinase (CK) levels
- increased ESR and C-reactive protein (CRP) levels
Several factors decrease the risk of malignancy :
- interstitial lung disease (ILD)
- inflammatory arthropathy
- Raynaud syndrome
- anti-Jo-1 antibody
Pathology
There is cell-mediated injury targeted at striated muscle with resultant atrophy, edema, coagulation necrosis, fibrosis and calcification.
Markers
- elevated muscle enzymes (e.g. CK)
- elevated muscle specific antibodies
- anti-RNA
- anti-Mi2
Subtypes
- hypomyopathic dermatomyositis
- clinically amyopathic dermatomyositis (CADM) / amyopathic dermatomyositis
Radiographic features
Plain radiograph
- typically shows dystrophic calcification in muscles and soft tissues (calcinosis universalis)
- sheet-like although at least four patterns have been described with childhood dermatomyositis
- classically seen affecting the thigh regions
- chest radiograph may show diaphragmatic elevation
- acro-osteolysis
Fluoroscopy
Barium swallow
- may show disordered peristalsis involving the upper esophagus i.e. the portion supplied by skeletal muscle
MRI
- T2: generally hyperintense signal throughout the affected muscles; calcific areas may be low signal; perimuscular edema may additionally appear as high signal; signal intensity may return to normal after treatment
Differential diagnosis
General imaging differential considerations include:
- polymyositis: does not affect the skin
Practical points
MRI T2-weighted sequences are useful to guide muscle biopsy:
- areas of edema related to the active inflammatory process
- non-specific end-stage fatty atrophic muscle should be avoided
Further imaging in the form of a contrast-enhanced CT of the chest, abdomen and pelvis may be undertaken to exclude an associated primary malignancy.
Siehe auch:
- Lungenkarzinom
- Akroosteolyse
- Interstitielle Lungenerkrankung
- Calcinosis cutis
- muskuloskelettale Manifestationen Dermatomyositis
und weiter:
- Sklerodermie Ösophagus
- inflammatorischer Pseudotumor der Orbita
- Systemische Sklerodermie
- gluteal injection site granuloma
- Amyloidose
- calcinosis circumscripta
- causes of pulmonary arterial hypertension
- radiologisches muskuloskelettales Curriculum
- Fibrodysplasia ossificans progressiva
- interstitial pneumonia
- subkutane Verkalkungen
- retikuläres Muster
- bilaterale axilläre Lymphadenopathie
- Myositis
- differential diagnosis of intramuscular high STIR signal on MRI
- dracunculiasis
- Rheuma Differentialdiagnose
- Muskelödem
- dystrophic calcification within the breast
- dystrophic soft-tissue calcification
- Bazex-Syndrom
- juvenile Dermatomyositis
- Merkspruch Weichteilverkalkungen

 Assoziationen und Differentialdiagnosen zu Dermatomyositis:
Assoziationen und Differentialdiagnosen zu Dermatomyositis: