femoral neck fracture




















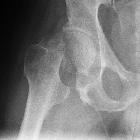


Neck of femur fractures (NOF) are common injuries sustained by older patients who are both more likely to have unsteadiness of gait and reduced bone mineral density, predisposing to fracture. Elderly osteoporotic women are at greatest risk.
Epidemiology
Incidence is increasing as the proportion of the elderly population in many countries increases . In patients aged between 65 and 99, femoral neck and intertrochanteric fractures occur with approximately the same frequency .
Pathology
Classification
Femoral neck fractures are a subset of proximal femoral fractures. The femoral neck is the weakest part of the femur.
Since disruption of blood supply to the femoral head is dependent on the type of fracture and causes significant morbidity, the diagnosis and classification of these fractures is important. There are three types:
- subcapital: femoral head/neck junction
- transcervical: midportion of femoral neck
- basicervical: base of femoral neck
Subcapital and transcervical fractures are considered intracapsular fractures. While there is disagreement in the literature as to whether basicervical fractures are truly intracapsular or extracapsular, they should usually be treated like extracapsular fractures .
Further, severity of a subcapital fracture is graded by the Garden classification of hip fractures.
Mechanism
Most commonly :
- falls in the elderly
- significant trauma (e.g. motor vehicle collisions) in younger patients
In elderly patients, the mechanism of injury various from falls directly onto the hip to a twisting mechanism in which the patient’s foot is planted and the body rotates. There is generally deficient elastic resistance in the fractured bone .
The mechanism in young patients is predominantly axial loading during high force trauma , with an abducted hip during injury causing a neck of femur fracture and an adducted hip causing a hip fracture-dislocation.
Radiographic features
Plain radiographs (sensitivity 93-98%) is the first-line investigation for suspected NOF fractures. In patients with a suspected occult NOF fracture, MRI (sensitivity 99-100%) is recommended by many institutions as the second-line test if available within 24 hours, with CT or nuclear medicine bone scan third-line . However, a recent study reports that thin-slice MDCT is as sensitive as MRI .
Plain radiograph
- Shenton’s line disruption: loss of contour between normally continuous line from medial edge of femoral neck and inferior edge of the superior pubic ramus
- lesser trochanter is more prominent due to external rotation of femur
- femur often positioned in flexion and external rotation (due to unopposed iliopsoas)
- asymmetry of lateral femoral neck/head
- sclerosis in fracture plane
- smudgy sclerosis from impaction
- bone trabeculae angulated
- nondisplaced fractures may be subtle on x-ray
Report checklist
- AP pelvis and lateral hip should be viewed because pelvic fractures can mimic clinical features of hip fracture
- trace Shenton’s line
- assess for symmetry, particularly note lesser trochanter (may indicate external rotation)
- bone trabeculae
- sclerosis
- smudge
Treatment and prognosis
Treatment of neck of femur fractures is important. Significant complications such as avascular necrosis and non-union are very common without surgical intervention. The treatment options include non-operative management, internal fixation or prosthetic replacement.
Internal fixation can be performed with multiple pins, intramedullary hip screw (IHMS), crossed screw-nails or compression with a dynamic screw and plate . Replacing the femoral head is achieved with either hemiarthroplasty and total hip arthroplasty.
The high morbidity and mortality associated with hip and pelvic fractures after trauma has been well documented. Prognosis is varied but is complicated by advanced age, as hip fractures increase the risk of death and major morbidity in the elderly .
The risk of avascular necrosis (AVN) depends on the type of fracture. The Delbet classification correlates with the risk of AVN :
- type 1 (transphyseal): ~90% risk of AVN
- type 2 (subcapital): ~50% risk of AVN
- type 3 (basicervical/transcervical): ~25% risk of AVN
- type 4 (intertrochanteric): ~10% risk of AVN
As a general rule, internal fixation is recommended for young, otherwise, fit patients with small risk for AVN. While prosthetic replacement is reserved for fractures with a high risk of AVN and the elderly .
See also
Siehe auch:
- Garden classification
- Osteoporose
- das Femur
- transzervikale Schenkelhalsfraktur
- laterale Schenkelhalsfraktur
- Stressfraktur des Schenkelhalses
- mediale Schenkelhalsfraktur
- Osteoid-Osteom Schenkelhals
- eingestauchte Schenkelhalsfraktur
- Schenkelhalsfraktur Pauwels
- osteoporotic fracture
und weiter:
- Garden classification of hip fractures
- idiopathische kindliche Hüftkopfnekrose
- Hüftkopfnekrose
- proximale Femurfrakturen
- Femurfraktur
- radiologisches muskuloskelettales Curriculum
- Hüftgelenk
- undisplaced fractured neck of femur
- impacted subcapital fracture of femoral neck
- fracture dislocation of the hip
- subcapital femoral neck fracture
- intracapsular neck of femur fracture

 Assoziationen und Differentialdiagnosen zu Schenkelhalsfraktur:
Assoziationen und Differentialdiagnosen zu Schenkelhalsfraktur:






