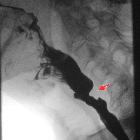
Gastro-esophageal reflux disease













Gastro-esophageal reflux disease (GERD) is a spectrum of disease that occurs when gastric acid refluxes from the stomach into the lower end of the esophagus across the lower esophageal sphincter (LES).
Epidemiology
It affects 10% to 20% of the adult population in the United States and Western countries .
Clinical presentation
Common clinical features in adults include epigastric and retrosternal burning sensations (heartburn or pyrosis), dysphagia, odynophagia, regurgitation leaving an acidic taste in the mouth, postural regurgitation (usually in the supine position), waterbrash (increased salivation), enamel erosions, and a chronic dry cough . Symptoms are particularly pronounced during the night .
In pediatrics, the presentation is often non-specific, with vomiting, upper and lower respiratory symptoms, irritability, aversion to food, and failure to thrive . A minority of pediatric patients with GERD (<1%) will additionally have spasmodic torticollis and dystonia, a constellation of symptoms known as Sandifer syndrome .
Pathology
Minor reflux disease
In most patients with reflux disease, reflux is initiated by transient collapses of LES pressure. This results in the lower end of the esophagus being bathed in gastric acid for longer than normal. Patients may be symptomatic without developing endoscopic appearances of esophagitis (40% of cases). These patients will also have no detectable abnormality on a barium swallow.
Loss of appropriate LES function gives rise to symptoms of reflux and globus symptoms, e.g. sensation of a lump at the back of the throat. It is affected by anatomical and physiological abnormalities:
- prolonged fundal distension
- sphincter shortening
- repetitive transient LES pressure collapse
Hiatus hernia
In normal patients, the intra-abdominal esophagus improves LES function. However, in patients with hiatus hernia, the amount of intra-abdominal esophagus is reduced and increases in intra-abdominal pressure are more likely to overcome the LES pressure and cause reflux.
Advanced reflux disease
In patients with a permanently low LES pressure, symptoms are generally more severe and there is evidence of disease in endoscopic or barium studies. Abnormalities that are radiologically detectable include:
- free reflux
- impaired primary peristalsis and poor clearance
- abnormal esophageal contractions
- esophagitis with scarring
- strictures, Barrett esophagus and aspiration
- sacculations and intramural pseudodiverticula
Theoretical response to acid
Traditional theories hold that GERD invokes a linear response of severity dependent on exposure to acid. Mild esophagitis progresses severe ulcerated esophagitis. This then progresses to Barrett esophagus and then, in a proportion of patients, dysplasia and eventually cancer develop.
Modern theory suggests that there is no such linear response to acid exposure in the lower osesophagus. Instead, the esophagus, under the stimulus of excess acid exposure, undergoes change in one of three ways:
Radiographic features
The difficulty in the radiographic diagnosis of GERD lies in the presence of spontaneous reflux on UGI examination in 20% of normal individuals, while some patients with pathologic GERD may present with reflux only after provocative maneuvers such as Valsalva, leg raising, and coughing .
Barium esophagograms
Findings associated with GERD include :
- gastroesophageal reflux (demonstrated with provocative maneuvers)
- hiatal hernia (associated with presence of reflux esophagitis)
- reflux esophagitis
- in more advanced cases, stricturing and/or esophageal shortening may be present
- impaired esophageal motility
Treatment and prognosis
Options include:
- medical treatment in minor cases with agents that inhibit gastric acid production
- surgery for advanced and resistant cases; fundoplication (for example Nissen-Rossetti, Dor or Toupet technique ) is the operation of choice, it can be done endoscopically or open surgery; a fold from the gastric fundus is wrapped around the lower esophageal junction to enforces the action of the sphincter
Siehe auch:
- Hiatushernie
- Magen
- Wandstarre unterer Ösophagus
- Ösophagus-pH-Metrie
- Antirefluxsysteme
- betontes pharyngoösophageales Segment
- gastrooesophagealer Reflux bei Kindern
- granular mucosal pattern of the oesophagus (differential)
- feline oesophagus
- hernioösophagealer Reflux
- Glykogenakanthose
und weiter:
- Cameron-Läsionen
- Zenker-Divertikel
- Diffuser Ösophagusspasmus
- Ösophagusbreischluck
- Zenker-Divertikel Grade nach Brombart
- Ösophagusstrikur
- Störungen der ösophagealen Peristaltik
- Ösophagitis
- Barsony-Pseudodivertikel
- Nussknackerösophagus
- peptische Ösophagusstenose
- His'scher Winkel
- Feline-Ösophagus
- abdominelle Manifestationen bei Mukoviszidose
- Fundoplikatio
- Odynophagie
- Nissen-Fundoplikatio
- tertiäre Peristaltik des Ösophagus
- Divertikel und Pouches des Pharynx

 Assoziationen und Differentialdiagnosen zu gastroösophageale Refluxerkrankheit:
Assoziationen und Differentialdiagnosen zu gastroösophageale Refluxerkrankheit: