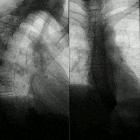
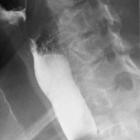
Ösophagusstrikur



















Esophageal stricture refers to any persistent intrinsic narrowing of the esophagus.
Pathology
Etiology
The most common causes are fibrosis induced by inflammatory and neoplastic processes. Because radiographic findings are not reliable in differentiating benign from malignant strictures, all should be evaluated endoscopically.
Upper and middle esophageal strictures
These most commonly result from:
- Barrett esophagus
- mediastinal radiation
- caustic ingestion
- congenital esophageal stenosis
- esophageal intramural pseudodiverticulosis
- skin diseases associated with mucosal ulceration, such as
- pemphigoid
- erythema multiforme
- epidermolysis bullosa dystrophica
Distal esophageal strictures
These are typically caused by gastro-esophageal reflux disease (GERD), either as a separate entity or in the setting of:
- scleroderma
- prolonged nasogastric intubation
- Zollinger-Ellison syndrome: high acidity reflux
- post partial or total gastrectomy: alkaline reflux
- performing the roux-en-Y procedure may avoid this, by diverting the pancreatic secretions and bile away from the gastric remnant
Associations
Esophageal strictures are often associated with a hiatal hernia.
Radiographic features
Benign strictures characteristically:
- smoothly tapering
- typically concentric narrowing, but may affect only one side of the esophagus (asymmetric wall rigidity)
Malignant strictures are characteristically:
- abrupt
- asymmetric
- eccentric with irregular, nodular mucosa
Tapered margins may occur with malignant lesions because of the ease of submucosal spread of a tumor.
Treatment and prognosis
The risk of Barrett esophagus in stricture is 20-40% and strictures should be evaluated endoscopically.
Benign esophageal strictures are typically treated with dilation, providing symptomatic relief, however recurrent strictures do occur. Complex strictures (length >2 cm, tortuous) are more likely to be recurrent. Treatment of malignant strictures involves treating the underlying cause. In palliative strictures, stent placement and brachytherapy play a role .
Siehe auch:
- Systemische Sklerodermie
- Tumoren des Ösophagus
- Intramurale Pseudodivertikulose des Ösophagus
- gastroösophageale Refluxerkrankheit
- Laugenverätzung Ösophagus
- kaustische Ösophagitis
- Säureverätzung Ösophagus
- Striktur des unteren Ösophagus
- Bolusimpaktation im Ösophagus
und weiter:

 Assoziationen und Differentialdiagnosen zu Ösophagusstrikur:
Assoziationen und Differentialdiagnosen zu Ösophagusstrikur: