malignancies of the pleura
 ähnliche Suchen
ähnliche Suchenmalignancies of the pleura
malignant pleural disease
malignant pleural thickening
pleural malignancies
Pleural malignancy
malignant pleural effusion
Malignancy of the pleura
Malignant pleural effusions
maligne pleurale Neoplasien
maligne Pleuratumoren
maligne Tumoren der Pleura
malignant pleural tumours
 siehe auch
siehe auchMalignant pleural disease usually heralds a poor prognosis, whether it represents a primary pleural malignancy or metastatic involvement.
Clinical presentation
Clinical presentation is variable. Patients may be asymptomatic or have pleuritic pain. If associated with a sizable pleural effusion, then respiratory compromise may be evident. If a tumor is from the chest wall, then musculoskeletal pain or even a palpable mass may be present.
Pathology
The pleura can be involved by malignancy by three main mechanisms:
In each of these, the manifestation can be either solid disease or a malignant pleural effusion, or a combination of both. The relative etiology is :
- metastatic carcinoma (e.g. primary lung): 58%
- mesothelioma: 28%
- non-Hodgkin lymphoma: 8%
- breast
- leukemia
- metastatic melanoma
- liposarcoma
- invasive thymoma
- rare primary pleural malignancies
- epithelioid angiosarcoma
- epithelioid hemangioendothelioma
- synovial sarcoma
- pleuropulmonary blastoma
- desmoplastic small round cell tumor of the pleura
Radiographic features
Conventional imaging is in general highly specific for the diagnosis of pleural malignancy but unfortunately lacks sensitivity .
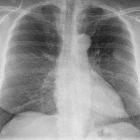
Plain radiograph
Plain films in the setting of malignant pleural effusion are insensitive at distinguishing it from a benign effusion. See malignant vs benign pleural effusion
In cases where multiple nodular regions or pleural thickening are present the diagnosis may be evident, especially if a primary tumor or other metastatic deposits are visible.
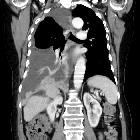
CT
CT is the work-horse of pleural imaging, able to achieve specificities of close to 100% . The portal-venous phase (also known as the pleural phase in the chest) is optimal for demonstrating pleural enhancement, rather than arterial phase imaging used routine thoracic CT. A number of features are recognized, including :
- circumferential pleural thickening
- nodular pleural thickening
- parietal pleural thickening greater than 1 cm
- mediastinal pleural involvement
- pleural calcification generally suggests a benign process
In many cases the primary malignancy will be visible (e.g. breast cancer, bronchogenic cancer) and/or evidence of pulmonary or bony metastases will be visible.
Nuclear medicine
FDG-PET is far more sensitive than conventional imaging in diagnosing malignant pleural disease and distinguishing them from benign processes . Hypermetabolism can be seen in either the pleura or pleural effusion. Although both benign and malignant processes, benign processes rarely increase the SUV over 2.0 .
MRI
MRI findings of high signal intensity on T2 in relation to intercostal muscles and/or contrast-enhanced on T1 images together with CT morphology has a 100% and a specificity of 93% in the detection of pleural malignancy .
Treatment and prognosis
Both treatment and prognosis are dependent on the underlying type of malignancy. In the case of primary malignancies of the pleura (e.g. mesothelioma) resection may be a possibility in highly selected cases.
Thoracentesis of malignant pleural effusions has limited effect with reaccumulation occurring, on average, at four days.
In general, and certainly in the case of diffuse pleural metastatic disease, systemic therapies or radiotherapy are the only options. These are discussed separately as part of articles pertaining to individual malignancies:
Differential diagnosis
Differential diagnosis depends on the predominant form the pleural disease takes:
- differential of nodular pleural thickening
- differential of a pleural effusion
- differential of a single pleural mass
Siehe auch:
- Pleuraerguss
- Pleurakarzinose
- benigne pleurale Tumoren
- Pleuramesotheliom
- pleurale Tuberkulose
- einzelne Pleuraraumforderung
- Tumoren der Pleura
- pleurale Metastasen
- Chondrosarkom der Pleura
- noduläre Pleuraverdickung
und weiter:
- Pleura
- einseitige Volumenminderung Thorax
- mesothelioma-like pleuropulmonary angiosarcoma
- Chondrom der Pleura
- Synovialsarkom der Pleura
- HiThoc
- desmoplastischer klein- und rundzelliger Tumor (DSRCT) der Pleura
- maligner solitärer fibröser Tumor der Pleura
- Pleuraverdickung
- Angiosarkom der Pleura
- diffuse Pleuraverdickung
 Assoziationen und Differentialdiagnosen zu malignant pleural thickening:
Assoziationen und Differentialdiagnosen zu malignant pleural thickening: