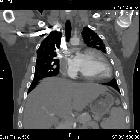
Pulmonalatresie



















Pulmonary artery atresia (or sometimes known as pulmonary atresia) is a congenital cardiovascular anomaly in which there is complete disruption between the right ventricular outflow tract (RVOT) and the pulmonary trunk.
Epidemiology
The estimated incidence is 1 in 10,000 births.
Pathology
The term pulmonary atresia can cover a broad spectrum of abnormalities depending on the extent of the disruption.
Classification
It can be classified into three types :
- pulmonary atresia with intact interventricular septum (PA-IVS)
- pulmonary atresia with VSD (PA-VSD)
- complex pulmonary atresia (pulmonary atresia with complex cardiac malformation)
Variants
Associations
- tetralogy of Fallot: PA-VSD is considered by some authors as a severe form of tetralogy of Fallot
- truncus arteriosus (Collett and Edwards type IV) or pseudotruncus: recognized to be a form of PA-VSD rather than truncus arteriosus
- heterotaxy syndrome: pulmonary atresia is present in two-fifths of right isomerism cases
Radiographic features
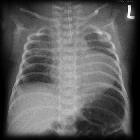
Plain radiograph
PA-VSD
- normal or mildly enlarged heart with poor or diminished pulmonary arterial vascular markings
- asymmetrical vascular suggests stenosis within pulmonary arterial tree
- there can be plethora due to horizontal arteries forming aortopulmonary collaterals
- mottled appearance as the lung periphery may suggest pleuro-pulmonary collateral formation
PA-IVS
- severe cardiomegaly from massive right atrial dilatation
Echocardiography
Echocardiography can characterize intracardiac anatomy. Has a limited role in assessing pulmonary artery anatomy.
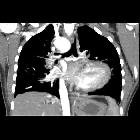
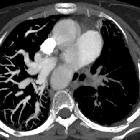
MDCT
MDCT is better than echocardiography for pulmonary artery anatomy. It allows evaluation of the following:
- length of pulmonary atresia
- presence of pulmonary artery confluence
- seagull appearance of the confluent pulmonary arteries and abbreviated pulmonary trunk
- size of main, right, and left pulmonary arteries at the origin and at the hilum
- presence of branch pulmonary artery stenosis
- sources of pulmonary blood flow to each lung, including the number of bronchopulmonary segments supplied by native pulmonary arteries and the distribution of major aortopulmonary collateral arteries (MAPCAs)
Cardiac MRI
Allows direct visualization of the anomaly. Cine sequences may show a dilated non contracting right ventricle . MR angiography allows detection of aortopulmonary collaterals and patent ductus arteriosus (if present).
Treatment and prognosis
- management varies depending on the presence of a VSD.
- one surgical technique includes the unifocalisation procedure which can be performed in cases with complete pulmonary artery atresia with major aortopulmonary collateral arteries (MAPCAs)
- prostaglandin E1 is used to keep the ductus open
Siehe auch:
- Fallot'sche Tetralogie
- tricuspid atresia
- Single Ventricle
- congenital cardiovascular anomaly
- unilaterale Pulmonalarterienatresie
und weiter:

 Assoziationen und Differentialdiagnosen zu Pulmonalatresie:
Assoziationen und Differentialdiagnosen zu Pulmonalatresie: