Persistierender Ductus arteriosus


































Patent ductus arteriosus or arteriosum (PDA) is a congenital cardiac anomaly where there is persistent patency of the ductus arteriosus, a normal connection of the fetal circulation between the aorta and the pulmonary arterial system that develops from the 6 aortic arch.
Epidemiology
Patent ductus arteriosus occurs in ~1 in 2000 full-term neonates with a F: M of 2:1 .
Clinical presentation
A large patent ductus arteriosus classically gives a loud continuous machine-like murmur.
Pathology
The ductus is a necessity in utero but usually undergoes functional closure 48 hours after birth. Patency of the ductus may be isolated or associated with other cardiac anomalies. In some circumstances, it is necessary to prolong life in patients with severe structural heart disease in whom a normal systemic circulation would be incompatible with life:
Non-cardiac associations
- prematurity
- surfactant deficiency
- trisomy 18
- trisomy 21
- rubella
Radiographic features
Plain radiograph
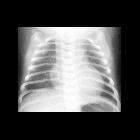
Chest radiographic features may vary depending on whether it is isolated or associated with other cardiac anomalies and with the direction of shunt flow (right to left or left to right). Can have cardiomegaly (predominantly left atrial and left ventricular enlargement if not complicated). Obscuration of the aortopulmonary window and features of pulmonary edema may be evident.
Echocardiography
Transesophageal and transthoracic echocardiography has been used to identify these lesions, assess for the presence of complications, and plan surgical intervention. Suspicion is often aroused when a measured shunt fraction (Qp: Qs) is > 1.0, consistent with a left-to-right shunt.
With transthoracic echocardiography, the parasternal short-axis view at the level of the aortic valve with color flow Doppler allows visualization of the flow through a patent ductus arteriosus. It classically appears as a high-velocity jet directed from the far-field toward the main pulmonary artery. Continuous-wave Doppler interrogation reveals continuous flow throughout systole and diastole. Larger lesions, especially with concomitant pulmonary hypertension, may demonstrate lower flow velocities and/or alternating flow direction.
The suprasternal notch view may also depict aliased, continuous flow from the proximal descending aorta toward the right pulmonary artery, visible under the aortic arch in the short-axis.
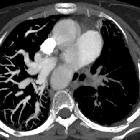
CT
MDCT can non-invasively provide detailed anatomical information .
Krichenko classification based on CT angiography:
- type A: conical ductus, prominent aortic ampulla with narrowing at pulmonary artery end
- type B: window, short and wide ductus with blending of pulmonary artery
- type C: long tubular ductus with no constrictions
- type D: multiple constrictions with complex ductus
- type E: elongated ductus with remote constriction
A ductus may have a tortuous morphology that does not fit in the Krichenko classification. This ductus type is usually observed in premature children and some authors proposed to classify it as type F or fetal type. Compared to types A to E, a type F ductus is larger, longer, tapers minimally from the aortic to pulmonary end, with a tortuous connection to the pulmonary artery giving a hockey-stick appearance .
Treatment and prognosis
- medical
- prostaglandin E1: to keep ductus open
- indomethacin: to close the ductus
- endovascular
- various closure devices
- surgical
- clipping or ligation to close
Complications
See also
Siehe auch:
- Down-Syndrom
- Fallot'sche Tetralogie
- Trisomie 18
- Ligamentum arteriosum
- persistierendes Foramen ovale
- Varianten der Herzanatomie
- hypoplastic left heart syndrome
- Surfactant-Mangelsyndrom
- Pulmonalatresie
- Eisenmenger-Reaktion
- Verkalkungen Ligamentum arteriosum
- persistierende fetale Zirkulation
und weiter:
- Anomalien des Aortenbogens
- Ektasie Aorta ascendens
- acute respiratory distress syndrome (ARDS)
- Herzfehler
- Kardiomegalie
- acyanotic congenital heart disease
- Transposition der großen Arterien
- Roberts-Syndrom
- causes of pulmonary arterial hypertension
- vergößerter linker Vorhof
- Ductus arteriosus
- CXR approach to congenital heart disease
- quadricuspid aortic valve
- Rubinstein-Taybi-Syndrom
- Noonan-Syndrom
- chest x-ray appeoach to congenital heart disease
- congenital heart disease - chest x-ray approach
- esophageal atresia with H-type tracheo-esophageal fistula
- pentalogy of Fallot
- H-type tracheo-oesophageal fistula with no atresia
- Agenesie des Perikards
- differential of an enlarged pulmonary trunk on chest radiography
- angeborene ösophagotracheale Fistel
- erweiterte Pulmonalarterie
- interrupted aortic arch (type A)
- Nicht-zyanotische Herzfehler
- Ductus arteriosus Aneurysma
- Diastolisches Aortenanzapfsyndrom
- Acute Respiratory Distress Syndrome neonatal

 Assoziationen und Differentialdiagnosen zu Persistierender Ductus arteriosus:
Assoziationen und Differentialdiagnosen zu Persistierender Ductus arteriosus:









