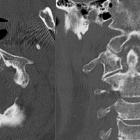
Retro-odontoid pseudotumor
Retro-odontoid pseudotumors, also known as periodontoid pseudotumors, are non-neoplastic soft tissue masses adjacent to the odontoid process (dens) of C2, which can cause cervicomedullary compression.
Epidemiology
The prevalence of retro-odontoid soft tissue thickening, particularly with mineralization presumed to represent calcium pyrophosphate deposition, increases significantly with age .
Clinical presentation
These are often asymptomatic. Acute inflammation in these masses (as in crowned dens syndrome) can manifest as neck pain or headache. As a chronic process, mass effect on the cervical spine can manifest as myelopathy including sensory and motor deficits.
Pathology
Pseudotumors can arise by various mechanisms and etiologies :
- atlantoaxial instability
- rheumatoid arthritis (in which case it may be termed pannus)
- trauma
- os odontoideum
- pigmented villonodular synovitis/tenosynovial giant cell tumor
- atlantoaxial hypermobility compensating for subaxial ankylosis
- deposition diseases
- calcium pyrophosphate dihydrate deposition disease (CPPD)
- hydroxyapatite deposition disease (HADD)
- gout
- amyloid arthropathy associated with hemodialysis
- dens fracture callus
- migrated disc herniation
Radiographic features
The entity is defined by soft tissue thickening at the atlantoaxial junction around the expected location of the transverse atlantic ligament, posterior to the dens.
CT
Mineralization within the pseudotumor may be present in calcium pyrophosphate deposition disease (chondrocalcinosis, linear/arciform), hydroxyapatite deposition disease (cloudlike), gout (faintly), fracture callus, and ossification of posterior longitudinal ligament (by definition).
Bony erosion may be present in rheumatoid arthritis, calcium pyrophosphate deposition disease, gout, and pigmented villonodular synovitis.
MRI
Signal characteristics vary by etiology. In general, there are no reliable imaging features that distinguish rheumatoid arthritis-related pannus from non-rheumatoid retro-odontoid pseudotumor.
- T1: usually low
- T2: variable, often heterogeneous
Differential diagnosis
Consider:
- retro-odontoid synovial cyst
- epidural hematoma
- epidural lipomatosis
See also
Siehe auch:

 Assoziationen und Differentialdiagnosen zu Pseudotumor hinter dem Dens:
Assoziationen und Differentialdiagnosen zu Pseudotumor hinter dem Dens: