Uterus septus











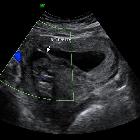






A septate uterus is a common type of congenital uterine anomaly, and it may lead to an increased rate of pregnancy loss. The main imaging differential diagnoses are arcuate uterus and bicornuate uterus.
Epidemiology
It is considered the commonest uterine anomaly (accounts for ~55% of such anomalies). It is classified as a class V Mullerian duct anomaly.
Septate uterus is the most common anomaly associated with subfertility, preterm labor, reproductive failure (67%), affecting ~15% of women with recurrent pregnancy loss .
Pathology
Septate uterus is considered a type of uterine duplication anomaly. It results from the partial or complete failure of resorption of the uterovaginal septum after fusion of the paramesonephric ducts. The septum is usually fibrous but can also have varying muscular components.
Subtypes
- a partial septum (subseptate uterus) involves the endometrial canal but not the cervix
- a septum is considered "complete" if it extends to either the internal or external cervical os
- septum extends into the vagina: septate uterus and vagina
Associations
As with other uterine anomalies, concurrent renal anomalies may be associated.
Radiographic features
General
- the external uterine fundal contour may be convex, flat, or mildly (< 1 cm) concave
- acute angle <75° between uterine cavities
- endometrial canals are completely separated by tissue isoechoic to myometrium with extension in the o endocervical canal
Hysterosalpingogram
Accuracy of hysterosalpingogram alone is only 55% for differentiation of septate uterus from the bicornuate uterus. An angle of less than 75° between the uterine horns is suggestive of a septate uterus, and an angle of more than 105° is more consistent with bicornuate uteri. Unfortunately, the majority of angles of divergence between the horns fall between these ranges, and considerable overlap between the two anomalies is noted.
Ultrasound
The echogenic endometrial stripe is separated at the fundus by the intermediate echogenicity septum. The septum extends to the cervix in a complete septate uterus. The external uterine contour must demonstrate a convex, flat, or mildly concave (ideally <1 cm) configuration and may best be appreciated on coronal images of the uterus.
May show vascularity in the septum in 70% of cases when assessed with color Doppler; and if present may be associated with a higher rate of obstetric complications .
MRI
MRI is considered the current imaging modality of choice.
On MR images, the septate uterus is generally normal in size and each endometrial cavity appears smaller than the configuration of a normal cavity.
The septum may be composed of fibrous tissue (low T2 signal intensity), myometrium (intermediate signal), or both .
Treatment and prognosis
The distinction between the septate uterus and bicornuate uterus has important management implications. The septum can be shaved off during hysteroscopy (metroplasty) to form a single uterine cavity without perforating the uterus .
The reproductive outcome has been shown to improve after resection of the septum, with reported decreases in the spontaneous abortion rate from 88% to 5.9% after hysteroscopic metroplasty.
Differential diagnosis
Considerations on hysterosalpingogram include:
- bicornuate uterus: the shape of the external uterine contour is crucial to differentiate a septate uterus from a bicornuate uterus because widely different clinical and interventional approaches are assigned to each anomaly
On ultrasound or MRI images also consider:
- arcuate uterus: small myometrial indentation in the fundus with normal fundal contour
- thick intrauterine adhesion band
Siehe auch:
und weiter:

 Assoziationen und Differentialdiagnosen zu Uterus septus:
Assoziationen und Differentialdiagnosen zu Uterus septus:

