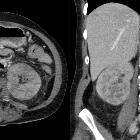
renal abscess
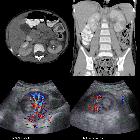
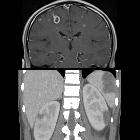
Renal abscess, is a collection of infective fluid in the kidney. It is usually a sequela of acute pyelonephritis, where severe vasospasm and inflammation may occasionally result in liquefactive necrosis and abscess formation.
Epidemiology
It can affect all ages and has no recognized gender predilection.
Risk factors
The predisposing factors include :
- diabetes mellitus
- renal calculi
- ureteral obstruction
Clinical presentation
The most common signs or symptoms are:
- fever
- flank/abdominal pain
- chills
- dysuria
Radiographic features
Ultrasound
Typically, a renal abscess appears as a well-defined hypoechoic area within the cortex or in the corticomedullary parenchyma. It demonstrates internal echoes within and an associated diffusely hypoechoic kidney due to acute pyelonephritis may be seen. Perinephric collection may also be seen.
CT
CT is currently the most accurate modality for diagnosis and follow-up of renal abscesses . An abscess appears as a well-defined mass of low attenuation with a thick, irregular wall or pseudo capsule, which can be better visualized on contrast enhanced scans. Gas within a low attenuation/cystic mass strongly suggests abscess formation. Renal parenchyma around the abscess cavity may appear hypoenhancing in nephrogram phase, and may appear hyperattenuating in delayed images. Associated fascial and septal thickening is seen with obliteration of perinephric fat.
In some cases, the formation of a discrete abscess is preceded by acute focal lobar nephronia which is a focal inflammation of the kidney without liquefaction. It appears as a solid mass.
Treatment and prognosis
Treatment consists of intravenous antibiotics and drainage, which may be performed under either ultrasound or CT guidance.
Complications
The main complication is abscess rupture, which can be described according to the space involved:
- calyceal system - pyonephrosis
- perinephric space - perinephric abscess
- anterior or posterior pararenal space beyond the perirenal fascia - paranephric abscess
- peritoneal cavity - subdiaphragmatic or pelvic abscess
These complications may lead to renal atrophy secondary to compression or obstruction.
Differential diagnosis
General imaging differential considerations include:
Siehe auch:
und weiter:

 Assoziationen und Differentialdiagnosen zu Nierenabszess:
Assoziationen und Differentialdiagnosen zu Nierenabszess: