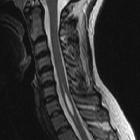
spinal epidermoid cyst



Spinal epidermoid cysts are cystic tumors lined by squamous epithelium. Unlike dermoid cysts, they do not contain skin appendages (hair follicles, sweat glands, sebaceous glands). They are usually extramedullary but rarely can be intramedullary. They may be congenital or acquired.
This article specifically relates to spinal epidermoid cysts. For a discussion of intracranial epidermoid cysts refer to the article: intracranial epidermoid cyst.
Epidemiology
Spinal epidermoid cysts are uncommon. They comprise between 0.5% and 1% of all spinal tumors but account for up to 10% of intraspinal tumors in children .
Unlike intracranial epidermoid cysts, which are almost always congenital in origin, most spinal epidermoid cysts are acquired. Although present since birth, congenital epidermoid tumors often do not present until the second to fourth decade of life . Males are more commonly affected than females.
Associations
Epidermoid cysts are commonly associated with spinal malformations such as spina bifida and hemivertebrae .
Clinical presentation
Spinal epidermoid cysts may be asymptomatic and discovered incidentally. If symptomatic, motor disturbances, pain, sensory disturbances, and bowel or bladder dysfunction may be present .
Pathology
Epidermoid cysts are benign. Histologically, they consist of stratified squamous epithelium supported by an outer layer of collagenous tissue. Progressive desquamation and breakdown of keratin from the epithelial lining into the interior of the cyst produce the characteristic content .
Congenital spinal epidermoids result from anomalous implantation of ectodermal cells during closure of the neural tube between the third and fifth week of embryonic life .
Acquired spinal epidermoids are a late complication of lumbar puncture, resulting from implanted epidermal elements into the spinal canal. The time interval between lumbar puncture and tumor diagnosis ranges from 1 to more than 20 years . Acquired spinal epidermoids are generally extramedullary and situated near a vertebral interspace . Prior to the introduction of styletted lumbar puncture needs, up to 40% of spinal epidermoid cysts were attributed to lumbar puncture. The incidence of this phenomenon has decreased significantly over the recent decades, but sporadic case reports still exist .
Radiographic features
Congenital epidermoids usually occur in the thoracic spine, particularly the congenital intramedullary form, and cauda equina. Acquired cysts are found in the lower lumbar region .
Plain radiograph
In advanced cases, there may be scalloping of the vertebral bodies or scoliosis .
CT
- well-circumscribed mass
- hypodense (similar to CSF)
- minimal to no enhancement
- calcification is rare
- potential osseous changes include an expanded spinal canal, laminar thinning and vertebral body scalloping
MRI
- well-defined lesion
- generally no perilesional edema
Although variable, typical signal characteristics include:
- T1: hypointense (similar to CSF)
- T2: hyperintense (similar to CSF)
- FLAIR: hyperintense compared to CSF
- T1 C+ (Gd): no enhancement or a thin rim of capsular enhancement
- DWI: bright (with corresponding low intensity on ADC map)
Signal intensity may be homogeneous or heterogeneous according to the variable water, lipid and protein composition of the cyst .
Treatment and prognosis
Spinal epidermoid cysts are slow growing. Surgery is the treatment of choice. Complete excision is usually possible and is curative . If the cyst wall is tightly adherent to the cord parenchyma, the wall should be left in place, however, this leads to a risk of recurrence .
Differential diagnosis
General imaging differential considerations include:
- spinal arachnoid cyst
- no restriction on DWI
- signal suppression on FLAIR
- vertebral anomalies uncommon
- spinal dermoid cyst
- usually contains fatty elements
- less likely to demonstrate diffusion restriction on DWI
- patients are usually younger than 20 years of age
- spinal neurenteric cyst
- thoracic and cervical regions most common
- usually ventral to spinal cord
- associated vertebral anomalies common
Also consider:
intramedullary spinal tumors or intradural extramedullary spinal tumors, depending on location.
Siehe auch:
- Ventriculus terminalis
- spinale Arachnoidalzyste
- Syringomyelie
- intramedulläre spinale Tumoren
- spinale Dermoidzyste
- intradurale extramedulläre Tumoren
und weiter:

 Assoziationen und Differentialdiagnosen zu spinale Epidermoidzyste:
Assoziationen und Differentialdiagnosen zu spinale Epidermoidzyste: