Tuberkulose des Peritoneums
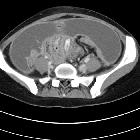






















Tuberculous peritonitis is a form of extrapulmonary tuberculosis affecting the peritoneum. It is frequently seen in association with other forms of gastrointestinal tuberculosis .
Epidemiology
Tuberculosis is usually confined to the respiratory system but may involve any organ system . Extrapulmonary manifestations may affect up to 15% of patients with tuberculosis. Risk factors for peritoneal involvement include concomitant HIV infection, patients who undergo peritoneal dialysis, and patients with cirrhosis .
The abdomen is the most common site of extrapulmonary tuberculosis, with peritoneal disease being the commonest form within the abdomen. Abdominal tuberculosis can also involve the solid organs, gastrointestinal tract, mesentery, and lymph nodes .
Pathology
Reactivation of tuberculous collections lying dormant in the peritoneum accounts for the majority of cases. Direct spread may occur from the gastrointestinal tract, and dissemination through lymphatic or hematogenous means have also been described. Direct extension from the female genital tract has been described .
Tuberculous peritonitis is commonly classified as follows:
- wet type
- most common (~90%)
- dry type
- fibrotic-fixed type
Of note, there is considerable overlap between the three types.
Tuberculosis in different organ systems may mimic alternate pathology so histopathological or laboratory evidence is often required to support suspicions on imaging before commencing treatment.
Radiographic features
CT
CT imaging features seen with tuberculous peritonitis include:
- nodular or symmetrical thickening of the peritoneum and mesentery
- abnormal peritoneal or mesenteric enhancement
- ascites
- enlarged hypodense lymph nodes: low attenuation lymphadenopathy
In addition, there can be more specific imaging features seen with individual types:
- wet type: exudative high attenuation ascites (20-45 HU), which may be free or loculated; high attenuation of the ascites is thought to be due to high protein and cellular content
- dry type: caseous mesenteric lymphadenopathy and fibrous adhesions; thickened, ‘cake-like’ omentum
- fibrotic type: omental ‘cake-like’ mass with fixed bowel loops; matted loops and mesentery with loculated ascites
The omental involvement may be ‘cake-like’, nodular, or smudged, but all appearances are similar to peritoneal carcinomatosis, which is the main differential diagnosis.
When the gastrointestinal tract is involved mural thickening of the ileocecal region is the most common site and can occur in conjunction with peritoneal involvement .
Ultrasound
- diffuse peritoneal thickening
- regular and hypoechoic enlargement of the parietal peritoneum common, may also demonstrate irregular/nodular pattern
- often hypervascular with color flow Doppler interrogation
- ascites
- often with interwoven thin fibrinous septations
- adhesions
- omental/mesenteric thickening
- great omentum may range in appearance from striated, with bands of alternating echogenicity, to nodular and hypoechoic
- increased bowel wall thickness
- lymphadenopathy
- early disease may demonstrate prominent mesenteric nodes with concomitant mesenteric thickening
- commonly involves retroperitoneal, peripancreatic, and periportal nodes
- echogenicity may be increased, or may contain central hypoechoic focus representing caseation
Differential diagnosis
On imaging (particularly CT), key differential considerations include:
Other less likely considerations include:
Siehe auch:
- Tuberkulose
- Peritonealkarzinose
- intraabdominelle Tuberkulose
- peritoneales Mesotheliom
- Tuberkulose des Peritoneums bei Kindern
- abdominelle tuberkulöse Lymphadenitis
und weiter:
- mesenteriale Pannikulitis
- omental cake
- pulmonale Tuberkulose
- Aszites
- Tumoren des Peritoneums
- Peritonitis
- extrapulmonale Manifestationen der Tuberkulose
- primary serous papillary carcinoma of the peritoneum
- peritoneal tuberculosis following infliximab therapy
- peritoneal tuberculosis: CT evaluation
- intra-abdominal abscess due to Mycobacterium Tuberculosis
- peritoneale Verkalkungen

 Assoziationen und Differentialdiagnosen zu Tuberkulose des Peritoneums:
Assoziationen und Differentialdiagnosen zu Tuberkulose des Peritoneums:







