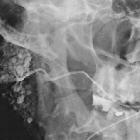
Warthin-Tumor
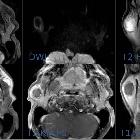












Warthin tumors, also known as lymphomatous papillary cystadenomas, are benign, sharply demarcated tumors of the salivary gland. They are of lymphoid origin and most commonly arise from parotid gland tail. They may be bilateral or multifocal in up to 20% of cases and are the most common neoplastic cause of multiple solid parotid masses.
Epidemiology
Warthin tumors are the 2 most common benign parotid tumor (after pleomorphic adenoma) and represent up to 10% of all parotid tumors. They are the commonest bilateral or multifocal benign parotid tumor. They typically occur in the elderly (6 decade), and twice as common in men (2.2:1) . Patients typically present with painless parotid swelling.
Morphology
They are often multicentric (20%) and are usually small (1-4 cm). They have a typically heterogeneous appearance on all modalities, often with cystic components (30%).
Location
Tends to favor the parotid tail region at the level of the mandibular angle.
In <10% cases, they are found elsewhere, including the submandibular glands, cervical lymph nodes, and ectopic nests of salivary tissue, e.g. larynx, maxillary antrum, oral cavity (e.g. lower lip, buccal mucosa) .
Associations
- smoking
- irradiation
Radiographic features
Has a greater tendency to undergo cystic change (~30%) than any other salivary gland tumor .
Ultrasound
Most tumors tend to be ovoid, with well-defined margins and multiple irregular, small, sponge-like anechoic areas . Tumors that are large (e.g. >5 cm) tend to have a higher proportion of cystic content than smaller lesions had and in some cases can be composed almost entirely of cystic material. They are often hypervascular.
CT
- classic appearance is a well-defined heterogeneous solid cystic lesion within the superficial lobe of parotid/parotid tail
- well defined
- no calcification
- cystic changes appear as intralesional lower attenuation
- moderate enhancement
- presence of mural nodule is strongly suggestive of Warthin tumor
- can be often seen bilaterally
MRI
Well defined and can be bilateral.
Signal characteristics
- T1: low to intermediate signal with cyst containing cholesterol components containing focal high signal
- T2: heterogeneous and variable signal intensity
- T1 C+ (Gd): cystic components do not take up contrast while solid parts usually enhance
Nuclear medicine
Often shows uptake with Tc-pertechnetate, thallium, and FDG-PET.
Treatment and prognosis
They are benign with an extremely low incidence of malignant transformation (~1%). Some advocate surgical excision while others favor conservative management with follow-up imaging. The commonest surgery is a superficial parotidectomy and recurrence rate is low, less than 5% in one of the largest published series .
Differential diagnosis
Possible imaging differential considerations include:
- pleomorphic adenoma
- other salivary gland tumors
- mucoepidermoid carcinoma
- adenoid cystic carcinoma (ACC)
- acinic cell carcinoma (of salivary gland)
- parotid nodal metastasis
- parotid non-Hodgkin lymphoma
- Sjogren syndrome
- benign lymphoepithelial lesions (BLEL) in HIV
- infiltrative lesion, e.g. sarcoidosis
Siehe auch:
- Sarkoidose
- Pleomorphes Adenom
- Glandula parotidea
- Parotistumoren
- Sjögren-Syndrom
- Adenoid-zystisches Karzinom
- mukoepidermoides Karzinom
- benigne lymphoepitheliale Läsionen
- acinic cell carcinoma
- parotid nodal metastasis
- parotid non hodgkin's lymphoma
und weiter:
- pleomorphes Adenom der Glandula parotis
- Tumoren der Speicheldrüsen
- zystische Läsionen der Glandula parotis
- Azinuszellkarzinom der Speicheldrüse
- Vergrößerung der Glandula parotis
- acinic cell carcinoma of salivary glands
- mukoepidermoides Karzinom der Speicheldrüsen
- salivary gland tumours showing uptake on Tc99
- Pleomorphes Adenom der Speicheldrüsen

 Assoziationen und Differentialdiagnosen zu Warthin-Tumor:
Assoziationen und Differentialdiagnosen zu Warthin-Tumor: