Paranasal sinus mucocele







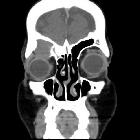


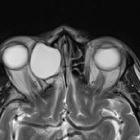




Paranasal sinus mucoceles represent complete opacification of one or more paranasal sinuses by mucus, often associated with bony expansion due to obstruction of the nasal sinus drainage.
Clinical presentation
Clinical presentation depends on two factors:
Mucoceles distort local anatomy and exert pressure on adjacent structures as they enlarge. Examples include:
- frontal mucocele extending into the front of the orbit, presenting as a mass
- posterior ethmoidal mucocele compressing the orbital apex
- sphenoidal mucocele extending posteriorly to impinge on the pituitary gland and brainstem
- maxillary mucocele may elevate the orbital floor with resultant proptosis
If a mucocele becomes infected, the clinical presentation is similar to acute sinusitis, with the potential extension of infection into adjacent spaces:
- intracranial: subdural empyema, meningitis, cerebral abscess
- orbit: subperiosteal abscess
- subcutaneous: e.g. Pott puffy tumor
Pathology
Mucoceles most likely occur as a result of obstruction of the ostium of a sinus due to inflammation, trauma, mass lesion, etc., with resultant accumulation of mucus and eventual expansion of the sinus. Some authors (the minority) believe that they represent a mucous retention cyst that gradually enlarges, eventually filling the whole sinus . Chronic non-invasive fungal sinusitis has also been associated with the formation of mucoceles . From a radiological point of view, which of these hypotheses is correct is immaterial.
The content of the mucocele is variable, and this impacts on the imaging appearances (see below). Most simple mucoceles are formed by clear thick mucus. If the mucocele has been infected (pyocele) then the content is similar to pus.
Location
The frontal sinus is particularly prone to developing mucoceles, and up to two-thirds of all mucoceles occur there. The ethmoidal sinuses are the next most common (~25%), whereas the maxillary and sphenoid sinuses are infrequently involved .
Subtypes (location specific)
- frontal mucocele
- frontoethmoidal mucocele
- ethmoid mucocele
- sphenoid sinus mucocele
- maxillary sinus mucocele
Associations
- cystic fibrosis: particularly if occurring in children
- paranasal sinus fibrous dysplasia: especially in frontal sinus
Radiographic features
Mucoceles are best imaged with a combination of CT (to assess bony changes) and MRI (to assess any extension into the orbit or intracranial compartment). The presence of air within an affected sinus rules out the possibility of a mucocele .
Plain radiograph
Skull radiographs do not have a significant role to play in the diagnosis of mucoceles. If obtained, they demonstrate opacification and expansion of the affected sinus.
CT
The affected sinus is completely opacified and the margins are expanded and usually thinned. Areas of complete bone resorption may be present, resulting in bony defect and extension of the 'mass' into adjacent tissues . Peripheral calcification is sometimes seen . Following administration of contrast, only peripheral enhancement (if any) is seen.
The content of the sinus is variable, depending on the degree of hydration, ranging from near-water attenuation to hyperattenuating as secretions become increasingly thick and desiccated .
MRI
MRI signal intensity is highly variable and depends on the proportions of water, mucus and protein :
- T1
- water-rich content: low signal (most common)
- protein-rich content: high signal
- T2
- water-rich content: high signal (most common)
- protein-rich content: low signal
- T1 C+ (Gd): enhancement, if present, only occurs at the periphery
- DWI: variable
NB: colonization with fungus can lead to very low signal on both T1 and T2 weighted sequences, mimicking a normal aerated sinus .
Treatment and prognosis
In general, drainage and marsupialisation of an affected sinus are sufficient. If large bony defects are present, reconstructive surgery may be necessary (e.g. of the orbital floor). If drainage remains impaired, the mucocele may recur.
Differential diagnosis
There is often little differential, if any, provided that contrast material has been administered. The differential includes:
- paranasal sinus tumors, e.g. inverted papilloma or sinonasal carcinoma
- most of these enhance
- mucus retention cyst
- does not completely fill the sinus
- no bony expansion
- antrochoanal polyp
- focally protrudes through the ostiomeatal complex
- acute sinusitis
- no bony expansion
- Aspergillus spp. infection
Siehe auch:
- akute Sinusitis
- antrochoanal polyp
- Mukozele Felsenbein
- Invertiertes Papillom
- abnormale Erweiterung Nasennebenhöhlen
- Noduläre Fasciitis der Nasennebenhöhlen
- Mukozele der Keilbeinhöhle
- spheno-ethmoidal mucocoele
- Mukozele Sinus maxillaris
- akute invasive fungale Sinusitis
und weiter:

 Assoziationen und Differentialdiagnosen zu Mukozele der Nasennebenhöhlen:
Assoziationen und Differentialdiagnosen zu Mukozele der Nasennebenhöhlen:



