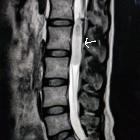
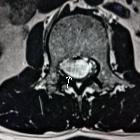
spinale Schwannome









































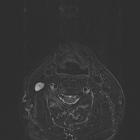
Spinal schwannomas are benign nerve sheath tumors within the spinal canal, typically arising from spinal nerve roots and it is the most common nerve sheath tumor of spine . They are one of the two most common intradural extramedullary spinal tumors, representing 15-50% of such lesions.
This article specifically relates to spinal schwannomas. For a general discussion of schwannomas, refer to the main article: schwannoma.
Epidemiology
They have a peak incidence in the fifth through seventh decades . There is no significant sex predilection.
Associations
The vast majority of spinal schwannomas are solitary and sporadic (95%) . However, there is an association with neurofibromatosis type 2 (NF2). In patients with NF2, almost all spinal nerve root tumors are schwannomas or mixed tumors. In a young adult without the NF2 mutation, the finding of multiple schwannomas may meet criteria for schwannomatosis.
Clinical presentation
As spinal schwannomas usually arise from the dorsal sensory roots, patients commonly present with pain. Radicular sensory changes also occur. Weakness is less common. Myelopathy may occur if the lesion is large.
Pathology
These tumors arise from schwann cells of sensory root and normally separated from other nerve roots. These are normally well defined, globular shape lesion with a capsule .
Radiographic features
Schwannomas are in most instances indistinguishable from neurofibromas. Refer to the article on spinal nerve sheath tumors for a discussion of their radiographic appearance.
The vast majority of spinal schwannomas are intradural extramedullary in location. Rarely (1%), intramedullary tumors are found .
They are most frequently seen in the cervical and lumbar regions, far more frequently than in the thoracic spine.
In general, schwannomas appear as solid, well-defined, rounded lesions, often with associated adjacent bony remodeling. When large, they may either align themselves with the long axis of the cord, forming sausage-shaped masses that can extend over several levels, or may protrude out of the neural foramen, forming a dumbbell-shaped mass.
MRI
Although neurofibromas and schwannomas can look identical, schwannomas are frequently associated with hemorrhage, intrinsic vascular changes (thrombosis, sinusoidal dilatation), cyst formation and fatty degeneration. These findings are rare in neurofibromas .
Signal characteristics include :
- T1: 75% are isointense, 25% are hypointense.
- T2: more than 95% are hyperintense, often with mixed signal
- T1 C+: virtually 100% enhance
An exception to the above signal characteristics is melanotic schwannomas, which are T1 hyperintense and T2 hypointense.
Treatment and prognosis
Schwannomas are slow growing lesions but can nevertheless be debilitating. They almost never undergo malignant change. Surgery is the treatment of choice. Gross total resection is usually curative for patients with sporadic tumors. For patients with NF2, there is a high incidence of new tumor formation.
Differential diagnosis
The main differentials are:
For a discussion of helpful distinguishing features, please refer to spinal nerve sheath tumors.
See also
Siehe auch:
- Schwannom
- Paragangliom
- spinal paraganglioma
- Neurofibrom
- Vestibularisschwannom
- neoplasms of the spinal canal
- spinal neurofibroma
- intradural extramedullary metastases
- intraspinales Meningeom
- benigner peripherer Nervenscheidentumor
- spinale Metastasen
- spinales Ependymom des Filum terminale
- Neoplasien der Cauda equina
- Schwannom der Cauda equina
- paraspinal mass
- schwannomatosis
- spinal nerve sheath tumours
- intradurale extramedulläre Tumoren
- Schwannome der Cauda equina bei Neurofibromatose Typ 2
- Schwannom der BWS
- schwannoma of the cervical spine
- Spinal nerve roots
- Jugular foramen (CN IX, X, XI)
und weiter:
- Myelonkompression
- genitourinary curriculum
- vertebrale Metastasen
- scalloping Wirbelkörper
- spinales Hämangioblastom
- spinal myxopapillary ependymoma
- spinales Ependymom
- paravertebrale Raumforderungen
- Myelopathie durch spinale Enge
- paraspinal ganglioneuroma
- intradural spinal mass lesions - an approach
- Sanduhrneurinom
- dumbbell appearance of spinal tumours
- neurilemmoma
- Schwannom der LWS
- Dumbbell schwannoma
- intrakraniale Schwannome
- cervical schwannoma
- widened neural canal

 Assoziationen und Differentialdiagnosen zu spinale Schwannome:
Assoziationen und Differentialdiagnosen zu spinale Schwannome: