myxopapillary ependymoma
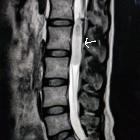

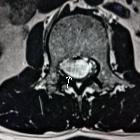






























Myxopapillary ependymomas are a variant type of ependymoma that occurs predominantly in the filum terminale and/or conus medullaris. They represent 13% of all spinal ependymomasand are the most common tumors of the cauda equina region.
Epidemiology
They tend to have an earlier clinical presentation than other spinal ependymomas, with a mean age of presentation of 35 years. There is a slight male predominance.
Clinical presentation
The most common presenting symptoms are low back, leg or sacral pain. Up to 25% of patients may present with leg weakness or sphincter dysfunction.
They may occasionally present as a subarachnoid hemorrhage .
Pathology
Etiology
They are thought to arise from the ependymal glia of the filum terminale.
Location
The vast majority are intradural and extramedullary spinal tumors, occurring in the lumbosacral spine involving the filum terminale and/or conus medullaris. Less commonly, they extend from the lumbar to the thoracic spine . Rarely, they can arise in the cervicothoracic spine or fourth ventricle .
Classification
These are WHO grade I ependymal tumors.
Macroscopic appearance
They are typically lobulated, encapsulated, and oval or sausage-shaped. They often have associated hemorrhage and may calcify or undergo cystic degeneration .
Microscopic appearance
Histologically, they contain papillary elements arranged radially around a hyalinized fibrovascular core, forming perivascular pseudorosettes, with myxoid material between the blood vessel and tumor cells . "Balloons" (rounded eosinophilic PAS positive structures) are sometimes encountered .
Immunophenotype
As is the case with ependymomas generally, myxopapillary ependymomas are GFAP, S100, and vimentin positive . CD99, AE1/AE3 and NCAM1 are also commonly positive .
Radiographic features
Plain radiograph / CT
If they become large, myxopapillary ependymomas may expand the spinal canal, cause scalloping of the vertebral bodies and extend out of the neural exit foramina.
MRI
They are well-defined intradural tumors. Classically, they present when larger and sausage-shaped, spanning more than one vertebral level, but small oval tumors are also seen. Smaller tumors tend to displace the nerve roots of the cauda equina; larger tumors often compress or encase them .
Signal characteristics
- T1
- usually isointense
- prominent mucinous component occasionally results in T1 hyperintensity
- hemorrhage and calcification can also lead to regions of hyper- or hypointensity
- T2
- overall high intensity
- low intensity may be seen at the tumor margins because of hemorrhage, called the cap sign (myxopapillary ependymomas are the subtype of ependymomas that are most prone to hemorrhage )
- calcification may also lead to regions of low T2 signal
- T1 C+ (Gd)
- enhancement is virtually always seen
- the enhancement pattern is typically homogeneous. However, they can have a variable enhancement pattern that, in part, depends on the amount of hemorrhage present
Treatment and prognosis
Myxopapillary ependymomas are generally slow-growing and benign. Occasionally, CSF dissemination occurs and multiple lesions are seen in 14-43% cases . Some sacral lesions are locally aggressive and metastasize to lymph nodes, lung, and bone. Aggressive behavior is more commonly seen in children .
They can often be excised completely. In these cases, the prognosis is excellent, with 5-year-survival over 98% .
If the tumor has extended to the conus medullaris, resection is often incomplete, with greater risk of local recurrence, and there is a greater risk of neurologic deficit .
Differential diagnosis
Differential diagnosis of a small conus and filum terminale myxopapillary ependymoma includes:
Differential diagnosis of a large myxopapillary ependymoma that causes sacral destruction:
- aneurysmal bone cyst: involving the spine
- chordoma
- giant cell tumor: involving the spine
See also
Siehe auch:
- Aneurysmatische Knochenzyste
- Chordom
- Ependymom
- Astrozytom
- Riesenzelltumor
- spinale Schwannome
- Cauda equina Lipom
- spinal paraganglioma
- spinales Ependymom
- spinales Ependymom des Filum terminale
- intradural spinal mass lesions - an approach
- spinale kavernomatöse Malformationen
- Neoplasien der Cauda equina
- ependymoma vs astrocytoma of the spinal cord
- intramedulläres Ependymom
und weiter:
- Schwannom
- WHO-Klassifikation der Tumoren des zentralen Nervensystems
- scalloping Wirbelkörper
- Superfizielle Hämosiderose der Leptomeningen
- neoplasms of the spinal canal
- spinales Hämangioblastom
- spinal myxopapillary ependymoma
- spinal nerve sheath tumours
- intraspinale Tumoren
- intradurale extramedulläre Tumoren
- spinal primitive neuroectodermal tumour
- malignant ependymoma
- Riesenzellependymom

 Assoziationen und Differentialdiagnosen zu spinal myxopapillary ependymoma:
Assoziationen und Differentialdiagnosen zu spinal myxopapillary ependymoma: