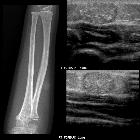
epidermal inclusion cyst





























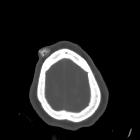




















Epidermal inclusion cysts or epidermal cysts are common cutaneous lesions that represent proliferation of squamous epithelium within a confined space in the dermis or subdermis.
Terminology
These are occasionally termed sebaceous cysts, although this is a misnomer as the lesion does not originate in the sebaceous glands. As such, the term epidermal inclusion cyst is preferred.
These are also called epidermoid cysts, which in turn are sometimes considered a type of dermoid cyst .
Clinical presentation
Epidermal cysts are either found incidentally or present as a firm non-tender lump. If they rupture a local inflammatory response to the necrotic debris released can mimic infection. Although they can be found anywhere, they are typically located on the scalp, face, neck, trunk, and back . Rarely they can be seen within bones representing an intraosseous epidermoid cyst .
Rarely epidermal cysts can undergo malignant degeneration with squamous cell carcinoma .
Pathology
They are thought to occur as a result of :
- traumatic/surgical implantation
- occlusion of the pilosebaceous unit
- congenital rests of cells
- human papillomavirus type 57 or 60 infections implicated palmoplantar epidermoid cysts
They are closely related to cholesteatomas, and should not be confused with epidermoid cysts of the CNS.
Radiographic features
On all modalities, they appear as well-circumscribed masses arising in or just deep to the skin.
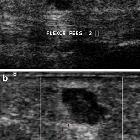
Ultrasound
Well-circumscribed predominantly hypoechoic mass. Typical shapes include :
- ovoid to spherical: ~70%
- lobulated: ~20%
- tubular: ~8%.
If small, it can mimic a typical anechoic cyst. Using subcutaneous fat as a reference, lesions tend to be hypoechoic. Larger lesions can be a little heterogeneous due to the presence of mucoid, fat, calcification or pus. Usually no associated vascularity. They, however, can have a variable appearance if ruptured, occasionally associated with vascularity and lobulated contours. On color Doppler, it may show twinkling artefact .
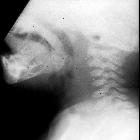
CT
The density of epidermal inclusion cysts is similar to that of water. The margins are usually slender and sclerotic.
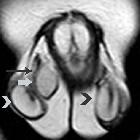
MRI
Imaging on MRI is similar to that of CNS epidermoid cysts or cholesteatomas, namely the content of the cyst is similar to CSF/water. In unruptured cases, typical signal characteristics include:
- T1: low/intermediate signal
- T2: high signal
- DWI
- some true restricted diffusion (similar to soft tissue on ADC)
- superimposed T2 shine through
- T1 C+ (Gd)
- no enhancement centrally
- may have thin peripheral enhancement
With ruptured cases, they may have septa, show thick and irregular rim enhancement, and can be accompanied by a fuzzy enhancement in surrounding subcutaneous tissues.
Treatment and prognosis
They are benign and generally do not require treatment. If infected they may require incision and drainage. If they continue to grow they may require excision.
Complications
- superimposed infection
- rupture
- concurrent occurrence of tumors within them, e.g. melanoma (very rare)
Differential diagnosis
General imaging differential considerations include:
- pilomatricoma
- ganglion cyst (if near a joint)
- neurogenic tumors e.g. neurofibroma
- nodular fasciitis
- myxoid tumors
- dermatofibrosarcoma protuberans
See also
Siehe auch:
- intrakranielle Epidermoidzyste
- Ganglion (Überbein)
- Neurofibrom
- Epidermoid in der Kalotte
- Dermatofibrosarcoma protuberans
- Epidermoidzyste Finger
- testicular epidermoid cyst
- intraventricular epidermoid
- Atherom Galea
- epidermale Inklusionszyste der Mamma
- Fasciitis nodularis
- Epidermoidzyste vs Dermoidzyste
- kutane Metastasen
- Malherbe-Tumor
- atheroma
- reifes zystisches Teratom
und weiter:
- Mega Cisterna magna
- Arachnoidalzyste
- Rathke Zyste
- Cholesteatom
- Epidermoidzyste
- ASP-Assoziation
- Pinealiszyste
- Ecchordosis physaliphora
- Gardner-Syndrom
- Tumor Kleinhirnbrückenwinkel
- Dermoidzyste
- Blake's-Pouch-Zyste
- Dandy-Walker continuum
- neuroglial cyst
- epidermale Inklusionszyste
- Keimzelltumor
- Akroosteolyse
- ependymal cyst
- erworbenes Cholesteatom
- Cholesteatom des äußeren Gehörgangs
- zystische Läsionen in der Hypophyse
- intraossäre Epidermoidzyste
- Steatocystoma multiplex
- hypothalamic lesions
- Dermoid Schädelkalotte
- testicular epidermoid
- congenital cholesteatoma
- white epidermoid
- periurethral cystic lesions
- Epidermoidzyste im Kleinhirnbrückenwinkel
- Epidermoid
- diffusionsgewichtete Bildgebung
- Galealipom
- Neoplasien der Cauda equina
- zystische Läsionen der Sellaregion
- Epidermoidzyste der Kalotte
- mostly / purely cystic pituitary region masses
- calcifying epithelioma of Malherbe
- mikrozystisches Meningeom
- diffusion MRI of an epidermoid tumor
- epidermoid cyst of the cauda equina
- Läsionen der Fingerspitze
- extratestikuläre intraskrotale Epidermoidzyste
- cystic extraaxial mass
- cutaneous epidermal cyst
- sutural epidermoid cyst
- Merkspruch Keimzelltumoren
- epidermale Inklusionszyste der Zunge
- Nasoalveoläre Zyste

 Assoziationen und Differentialdiagnosen zu epidermale Inklusionszyste:
Assoziationen und Differentialdiagnosen zu epidermale Inklusionszyste: