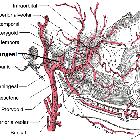
Nervus facialis












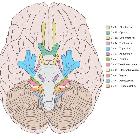




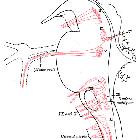

The facial nerve is one of the key cranial nerves with a complex and broad range of functions.
Although at first glance it is the motor nerve of facial expression which begins as a trunk and emerges from the parotid gland as five branches (see facial nerve branches mnemonic), it has taste and parasympathetic fibers that relay in a complex manner.
The facial nerve is the only cranial nerve that may show normal post-contrast enhancement, although this applies only to the labyrinthine segment up to the stylomastoid foramen. Enhancement of the other segments of the facial nerve and other cranial nerves is considered pathologic. Refer to normal facial nerve enhancement on MRI for more information.
Gross anatomy
Nuclei and brainstem tracts
Four cranial nerve nuclei contribute to the facial nerve: one motor, one secretomotor, and two sensory:
- facial nucleus
- in the ventrolateral pontine tegmentum, giving off fibers that loop posteriorly over the abducens nerve nucleus, which together form the facial colliculus in the floor of fourth ventricle
- supplies motor fibers to the stapedius and muscles of facial expression
- superior salivary (salivatory) nucleus
- in the pons, lateral to the facial nucleus
- supplies secretomotor parasympathetic fibers to lacrimal, submandibular, and sublingual glands
- nucleus of tractus solitarius (solitary nucleus)
- in the medulla and lower pons, lateral to the dorsal nucleus of the vagus nerve
- receives taste fibers from the anterior tongue via the chorda tympani
- spinal nucleus of the trigeminal nerve
- in the upper cervical spinal cord, medulla, and pons, ventral to the vestibular and cochlear nuclei
- receives somatosensatory fibers from the posterior external auditory canal
General course
The facial nerve has six named segments (facial nerve segments mnemonic):
Intracranial (cisternal) segment
The nerve emerges from lower lateral pons, lateral and rostral to the abducens nerve, and medial and caudal to the vestibulocochlear nerve (CN VIII) . It is joined by the nervus intermedius, which emerges lateral to the main trunk. Together the two travel laterally through the cerebellopontine angle to the internal acoustic meatus. The cisternal segment has no branches.
Meatal (canalicular) segment
Having been joined by the nervus intermedius, they are located in the anterior superior quadrant of the internal auditory canal, above the falciform crest and anterior to Bill bar. The meatal segment has no branches.
Labyrinthine segment
As the facial nerve and nervus intermedius pass through the anterior superior quadrant of the internal acoustic meatus it enters the Fallopian canal, passing anterolaterally between and superior to the cochlea (anterior) and vestibule (posterior), and then bends posteriorly (the anterior or first genu) at the geniculate ganglion (where the nervus intermedius joins the facial nerve and where fibers for taste synapse - see function below). It is here that two branches originate:
Some fibers contributing to the lesser petrosal nerve of the glossopharyngeal nerve also arise from the geniculate ganglion, but the nerve is described as a branch of the glossopharyngeal nerve rather than the facial nerve.
The labyrinthine segment is the shortest only measuring 3-4 mm. It is also the narrowest and the most susceptible to vascular compromise (see blood supply below).
Tympanic segment
As the nerve passes posteriorly from the geniculate ganglion it becomes the tympanic segment (8-11 mm in length) and is immediately beneath the lateral semicircular canal in the medial wall of the middle ear cavity. The bone of the Fallopian canal is often dehiscent in the area of the oval window in 25-55% of postmortem specimens, having mucosa in direct contact with the nerve. The nerve passes posterior to the cochleariform process, tensor tympani, and oval window. Just distal to the pyramidal eminence the nerve makes a second turn (posterior or second genu) passing vertically downwards as the mastoid segment. The tympanic segment has no branches.
Mastoid segment
The mastoid segment, measuring 8-14 mm in length, extends from the posterior genu to the stylomastoid foramen, through what is confusingly referred to as the Fallopian canal. It runs in the medial wall of the aditus ad antrum of the mastoid posterior to the facial recess of the mesotympanum. It gives off three branches:
- nerve to stapedius
- chorda tympani: terminal branch of the nervus intermedius carrying both secretomotor fibers to the submandibular gland and sublingual gland and taste to the anterior two-thirds of the tongue
- nerve from the auricular branch of the vagus nerve (CN X): pain fibers to the posterior part of the external acoustic meatus hitchhike from the jugular foramen
Extratemporal segment
As the nerve exits the stylomastoid foramen, it gives off the posterior auricular nerve that supplies part of the external acoustic meatus, tympanic membrane, auricular muscles, and occipital part of occipitofrontalis. It then passes between the posterior belly of the digastric muscle and the stylohyoid muscle, supplying both and the enters the parotid gland. Lying between the deep and superficial lobes of the gland the nerve divides into two main branches at the pes anserinus (Latin: duck foot) - superior temporofacial and inferior cervicofacial branches. From the anterior border of the gland, five branches emerge (from superior to inferior):
- temporal (which should not be confused with the deep temporal nerves of the mandibular division of the trigeminal nerve)
- zygomatic (which should not be confused with the zygomatic nerve of the maxillary division of the trigeminal nerve)
- buccal (which should not be confused with the buccal nerve of the mandibular division of the trigeminal nerve)
- mandibular (marginal) (which should not be confused with the mandibular division of the trigeminal nerve)
- cervical
See facial nerve branches mnemonic here.
The temporal branch runs with the superficial musculoaponeurotic system (SMAS) over the zygomatic arch. This branch is at risk during surgery in this region. To avoid damage procedures should be deep to the SMAS (e.g. zygomatic fracture repairs).
The mandibular branch, in 80% of cases, runs along the lower border of the mandible (thus also referred to as marginal branch). In 20% of cases however it can be up to 2 cm below the margin of the mandible. It is crucial to be aware of this if surgery in the submandibular region is being performed. Injury to this branch will result in paralysis of mouth depressors.
Function
Taste
Taste fibers to the anterior two-thirds of the tongue originate in the nucleus of the tractus solitarius (NTS), travel in the nervus intermedius (preganglionic) where they join the facial nerve at the geniculate ganglion and synapse. Postganglionic fibers travel with the facial nerve and are given off as the chorda tympani, which eventually joins the lingual nerve (branch of the trigeminal nerve (CN V)).
Parasympathetic
Preganglionic fibers originate in the superior salivary nucleus and join the facial nerve at the geniculate ganglion having traveled with the nervus intermedius. They do not synapse in the ganglion, but rather pass through to be distributed between:
Somatic motor
The muscles of facial expression are supplied by the branches of the terminal facial nerve.
Blood supply
The facial nerve receives its arterial supply from three main sources:
The labyrinthine segment is the most vulnerable to ischemia as the connections between the labyrinthine artery and superficial petrosal artery are very tenuous, with each artery essentially being end arteries.
Related pathology
Disruption or compromise of the nerve leads to facial palsy.
Bilateral conditions
- Melkersson-Rosenthal syndrome
- Möbius syndrome
- Guillain-Barré syndrome
- leprosy
- HIV infection-related facial nerve palsy: may precede seroconversion
Unilateral conditions
- congenital facial palsy
- Bell palsy
- sarcoidosis & other granulomatous disorders
- infection
- leprosy: especially with paralysis of upper face
- chronic otomastoiditis
- Lyme disease
- HIV infection-related facial nerve palsy
- herpes zoster (Ramsay Hunt syndrome)
- neoplasm(s) and masses
- facial nerve schwannoma
- facial nerve hemangioma
- facial nerve choristoma
- CNS lesions
- perineural spread especially from head and neck squamous cell carcinoma and adenoid cystic carcinoma of the parotid gland
- compression from vestibular schwannoma
- trauma: especially temporal bone fractures
- cardiofacial syndrome: typically lower lip or complete facial palsy
- familial facial palsy
Siehe auch:
- Cavum tympani
- Nervus trigeminus
- Sarkoidose
- chronische Otomastoiditis
- Glandula parotidea
- Nervus vestibulocochlearis
- Cochlea
- Hirnnerven
- tongue
- Trommelfell
- Anatomie Hirnstamm
- sublingual gland
- Vestibularisschwannom
- superior salivary nucleus
- Guillain-Barré-Syndrom
- Adenoid-zystisches Karzinom
- internal acoustic meatus
- labyrinthine artery
- vierter Ventrikel
- Nervus glossopharyngeus
- facial colliculus
- Glandula submandibularis
- Foramen jugulare
- Arteria occipitalis
- Musculus digastricus
- Ganglion pterygopalatinum
- Musculus stylohyoideus
- cerebellopontine angle
- Arteria cerebelli anterior inferior
- Jochbogen
- Meatus acusticus externus
- Lepra
- submandibular ganglion
- idiopathische Facialisparese
- nerve to stapedius
- Nervus petrosus minor
- Moebius syndrome
- Ganglion oticum
- Nucleus salivatorius inferior
- facial nerve haemangioma
- Mandibula
- congenital facial palsy
- Lyme-Borreliose
- facial nerve choristoma
- Ramsay-Hunt Neuralgie
- Processus cochleariformis
- Tränendrüse
- Jochbogenfraktur
- Schwannom des Nervus facialis
- Crista verticalis superior (Bill's bar)
- vestibule of the ear
- Frakturen Os temporale
- head and neck SCC
- falciform crest
- Arteria meningea media
- Ganglion geniculi
- nervus intermedius
- stylomastoid foramen
- Canalis nervi facialis
- perineural spread
- tympanic plexus
- Fenestra vestibuli
- pyramidal eminence
- stylomastoid artery
- Nervus petrosus major
- lateral semicircular canal
- nucleus of the tractus solitarius (NTS)
- greater superfical petrosal nerve
- superficial petrosal artery
- superficial musculoaponeurotic system (SMAS)
- Nervus lingualis
- Nervus petrosus externus
- HIV infection related facial nerve palsy
- tensor tympani
- mnemonic here
und weiter:
- facial nerve branches (mnemonic)
- Tumor Kleinhirnbrückenwinkel
- juvenile maligne Osteopetrose
- Nervus abducens
- Musculus buccinator
- möbius syndrome
- zerebellopontines Lipom (Lipom im Kleinhirnbrueckenwinkel)
- Pes anserinus
- Melkersson-Rosenthal syndrome
- facial colliculus syndrome
- vertebrobasiläre Dolichoektasie
- internal auditory canal nerves (mnemonic)
- facial nerve segments (mnemonic)
- Felsenbein-Querfrakturen
- Neuritis Nervus facialis
- falciform crescent
- Fazialisparese
- Hirnnerven Eselsbrücke
- facial and vestibulocochlear nerves: normal MRI appearance
- Parotidektomie
- Michel-Aplasie
- persistierende Arteria stapedia
- Arterien von Kopf und Hals
- MR imaging of facial nerve in a case of Bell's palsy
- chvostek sign
- Dehiszenz des Canalis nervi facialis

 Assoziationen und Differentialdiagnosen zu Nervus facialis:
Assoziationen und Differentialdiagnosen zu Nervus facialis: