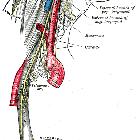
Paragangliome von Kopf und Hals






Paragangliomas of the head and neck are rare, representing <0.5% of all head and neck tumors. They arise in a number of locations along the carotid sheath and middle ear including the carotid bifurcation, vagal ganglia, jugular bulb, and tympanic plexus.
For a general discussion of the pathology of these tumors please refer to the paraganglioma article.
Epidemiology
Overall there is a 3:1 female predominance. Two-thirds of cases are diagnosed between the ages of 40 and 60. Approximately 25% are multicentric, and these tend to be familial.
Clinical presentation
Clinical presentation will depend on location.
When involving the middle ear cavity, the tumor may grow large and extend into the external ear: these may present with pulsatile tinnitus, cranial nerve palsies (typically IX-XI, Vernet syndrome), or conductive hearing loss. Direct otoscopic examination may reveal a retrotympanic vascular mass.
In the neck, the patient may present with a local mass.
Pathology
Paragangliomas arise from neural crest cells, which can differentiate into cells of either the parasympathetic or sympathetic nervous system. In the head and neck, paragangliomas tend to be innervated by the parasympathetic system and do not secrete catecholamines and are thus termed nonchromaffin paragangliomas .
Multiple paragangliomas (both sporadic and familial subtypes) are commonly associated with mutations of the succinate dehydrogenase subunit genes .
Associations
Although often sporadically identified in otherwise normal individuals, paragangaliomas are seen associated with a number of systemic conditions including :
- multiple endocrine neoplasia (MEN)
- neurofibromatosis type 1 (NF1)
- paraganglioma syndrome
- succinate dehydrogenase mutations
- von Hippel-Lindau syndrome (vHL)
Location
They are divided according to location:
- carotid body tumor (or chemodectoma)
- located at the carotid body, and splaying the carotid bifurcation
- most common paraganglioma of the head and neck (60-67% of total)
- glomus tympanicum tumor
- arise from the glomus tympanicum
- confined to the middle ear overlying the cochlear promontory
- arises from the inferior tympanic branch of glossopharyngeal nerve (CN IX) (or Jacobson's nerve)
- second most common head and neck paraganglioma
- glomus jugulotympanicum tumor
- arising from the glomus jugulotympanicum
- extending between the cochlear promontory and jugular foramen
- arising from Arnold's nerve, the mastoid branch of the vagus nerve (CN X)
- glomus jugulare tumor
- arising from the glomus jugulare
- confined to the jugular foramen
- extending into the middle ear
- glomus vagale tumor
- arising from the glomus vagale associated with vagus nerve (CN X)
- least common head and neck paraganglioma
Radiographic features
CT
- useful when bone erosion occurs
- a moth-eaten pattern is typical
MRI
- T1: may show a “salt and pepper” appearance; salt representing blood products from hemorrhage (uncommon) and pepper representing flow voids due to high vascularity (common)
- T1C+ (Gd): demonstrate rapid wash-in and wash-out (as opposed to the more slow and steady enhancement of a schwannoma)
Angiography
- intense tumor blush
- the most common feeding vessel is the ascending pharyngeal artery
Scintigraphy
- high uptake on In labeled octreotide
Treatment and prognosis
Treatment is usually by excision. Preoperative endovascular embolization is often used to reduce tumor vascularity and aid excision. Radiotherapy may be used for palliation of unresectable lesions.
Malignant transformation is not terribly uncommon and has been reported in 16-19% of glomus vagale tumors, in 6% of carotid body tumors, and in 2-4% of glomus tympanicum tumors.
Differential diagnosis
When completely imaged with CT and contrast-enhanced MRI usually little differential is present. During work-up, however, numerous entities should be considered.
In the middle ear/petrous temporal bone consider:
- cholesterol granuloma
- cholesteatoma
- metastasis
- meninigoma
- base of skull tumors
In the jugular and carotid region consider:
- jugular schwannoma
- lymph node metastasis/mass
Siehe auch:
- Cavum tympani
- Glomus caroticum Tumor
- Glomus jugulare Tumor
- Paragangliom
- Phäochromozytom
- spinal paraganglioma
- Nervus glossopharyngeus
- glomangioma
- carotid body
- Foramen jugulare
- carotid bifurcation
- glomus tympanicum tumour
- pulssynchrones Ohrgeräusch
- glomus body
- Glomustumor am Finger
- Paragangliom des Nervus vagus
- non chromaffin paraganglion cells
- Vernet's syndrome
- glomus jugulare: imaging and pre-operative embolization
- Zuckerkandl-Organ
- Jacobson-Anastomose
- salt and pepper
- nonchromaffin paraganglion cells
- Arnold nerve
und weiter:

 Assoziationen und Differentialdiagnosen zu Paragangliome von Kopf und Hals:
Assoziationen und Differentialdiagnosen zu Paragangliome von Kopf und Hals: