renal angiomyolipoma
















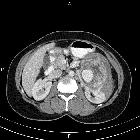





































 nicht verwechseln mit: Myelolipom der Niere
nicht verwechseln mit: Myelolipom der NiereRenal angiomyolipomas (AML) are a type of benign renal neoplasms encountered both sporadically and as part of a phakomatosis, most commonly tuberous sclerosis. They are considered one of a number of tumors with perivascular epitheloid cellular differentiation (PEComas) and are composed of vascular, smooth muscle and fat elements. They can spontaneously hemorrhage, which may be fatal. AMLs usually have characteristic radiographic appearances.
Epidemiology
Angiomyolipomas are the most common benign solid renal lesion and also the most common fat-containing lesions of the kidneys. The majority of angiomyolipomas are sporadic (80%) and are typically identified in adults (mean age of presentation 43 years), with a female predilection (F:M of 2-4:1).
The remaining 20% are seen in association with phakomatoses, the vast majority in the setting of tuberous sclerosis (80% of them get AML) although they have also been described in the setting of von Hippel-Lindau syndrome (vHL) and neurofibromatosis type 1 (NF1) . In these cases, they present earlier (usually identified by the age of 10 years), are larger, and are far more numerous. They are more likely to be fat-poor which accounts for their earlier presentation . They have also been associated with lymphangioleiomyomatosis (LAM).
Clinical presentation
Angiomyolipomas are often found incidentally when the kidneys are imaged for other reasons, or as part of screening in patients with tuberous sclerosis.
Symptomatic presentation is most frequently with spontaneous retroperitoneal hemorrhage; the risk of bleeding is proportional to the size of the lesion (>4 cm diameter). Shock due to severe hemorrhage from rupture is described as Wunderlich syndrome .
Patients may present with numerous other symptoms and signs , e.g. palpable mass, flank pain, urinary tract infections, hematuria, renal failure, or hypertension .
Pathology
Angiomyolipomas are members of the perivascular epithelioid cells tumor group (PEComas) and are composed of variable amounts of three components; blood vessels (-angio), plump spindle cells (-myo) and adipose tissue (-lipo).
Almost all classic angiomyolipomas are benign but they do have the risk of rupture with bleeding or secondary damage/destruction of surrounding structures as they grow.
Variants
Two histological types have been described
- typical (triphasic)
- atypical (monophasic or epithelioid)
A special variant called an epithelioid angiomyolipoma is composed of more plump, epithelial-looking cells, often with nuclear atypia, that have a described risk of malignant behavior. This variant, unlike conventional AMLs, may mimic renal cell carcinoma . Metastases have also been described .
Radiographic features
The cornerstone of diagnosis on all modalities is the demonstration of macroscopic fat, however in the setting of hemorrhage, or when lesions happen to contain little fat, it may be difficult to distinguish an angiomyolipoma from a renal cell carcinoma.
In tuberous sclerosis the lesions are larger than isolated AML and often multiple and bilateral.
Ultrasound
- tend to appear as hyperechoic lesions on ultrasound, located in the cortex and with posterior acoustic shadowing
- in the setting of tuberous sclerosis, they may be so numerous that the entire kidney is affected, appearing echogenic with the loss of normal corticomedullary differentiation
- contrast-enhanced ultrasound
- tend to enhance peripherally
- decreased central enhancement, compared with normal cortex
CT
Most lesions involve the cortex and demonstrate macroscopic fat (less than -20 HU). When small, volume averaging may make differentiation from a small cyst difficult. It is essential to remember that rarely renal cell carcinomas (RCC) may have macroscopic fat components and as such the presence of fat is strongly indicative of an angiomyolipoma, but not pathognomonic.
It is important to realize that ~5% of angiomyolipomas are fat-poor . This is especially the case in the setting of tuberous sclerosis, where up to a third do not demonstrate macroscopic fat on CT . Absence of ossification/calcification on imaging is in favor of AML .
MRI
MRI is excellent at evaluating fat-containing lesions, and two main sets of sequences are employed. Firstly, fat-saturated techniques demonstrate high signal intensity on non-fat-saturated sequences and loss of signal following fat saturation.
The second method is to use in-phase and out-of-phase imaging, which generates India ink artifact at the interface between fat and non-fat components. This can occur either at the interface between the angiomyolipoma and surrounding kidney or between fat and non-fat components of the mass . Chemical shift signal intensity loss, along with other features, may suggest a fat-poor AML .
Digital subtraction angiography (DSA)
Angiomyolipomas are hypervascular lesions demonstrating often characteristic features:
- arterial phase: a sharply marginated hypervascular mass with a dense early arterial network, and tortuous vessels giving the "sunburst" appearance
- venous phase: whorled "onion peel" appearance of peripheral vessels
- micro- or macro-aneurysms
- absent arteriovenous shunting
Treatment and prognosis
Angiomyolipomas found incidentally usually require no therapy (when small), although follow-up is recommended to assess for growth. Small solitary AMLs (<20 mm) probably do not require follow-up due to their slow growth .
Larger AMLs, or those that have been symptomatic, can be electively embolized and/or resected with a partial nephrectomy.
The traditional convention is that intervention is considered when an angiomyolipoma reaches 40 mm in size .
Lesions that present with retroperitoneal hemorrhage often requires emergency embolization as a life-saving measure.
mTOR inhibitors (e.g. everolimus) have been shown to significantly decrease AML size and may help to preserve renal function in tuberous sclerosis patients.
Differential diagnosis
When an AML has typical appearances there is essentially no differential. If atypical, especially when fat-poor, other lesions to consider include:
- renal cell carcinoma (RCC)
- macroscopic fat in RCC almost always occurs in the presence of ossification/calcification
- focal or diffuse signal loss in opposed phase suggests microscopic fat (in contrast to the curvilinear India ink artifact seen with macroscopic fat), which is very common in clear cell renal cell carcinoma and less common in fat-poor AML
- retroperitoneal liposarcoma invading the kidney:
- presence of a large vessel extending into the renal cortex suggestive of AML; liposarcoma is hypovascular
- renal parenchymal defect at the site of tumor contact favors exophytic angiomyolipoma - claw sign
- calcifications suggest liposarcoma
- oncocytoma: may contain fat
- Wilms tumor: may contain fat
- adrenal myelolipoma
- perirenal fat entrapment / renal junctional parenchymal defect
Siehe auch:
- Angiomyolipom
- Myelolipom Nebenniere
- Nierenzellkarzinom
- Tuberöse Sklerose
- Lymphangioleiomyomatose
- retroperitoneales Liposarkom
- Nephroblastom
- Onkozytom
- benigne Nierentumoren
- Angiomyolipom Nebenniere
- Renal replacement lipomatosis
- eingeblutetes Angiomyolipom
- aggressives Angiomyolipom
- Myelolipom der Niere
- Sinuslipomatose der Niere
- Lipom der Niere
und weiter:
- Neurofibromatose Typ 1
- Myelolipom
- Morbus Hippel-Lindau
- Wunderlich-Syndrom
- claw sign
- pädiatrische Nierentumoren
- extraadrenales Myelolipom
- Angiomyolipome der Niere bei tuberöser Sklerose
- Embolisation Angiomyolipom der Niere
- bilateral giant renal angiomyolipomas
- renal cell carcinoma and multiple angiomyolipomas in a patient with tuberous sclerosis
- pulmonary lymphangioleiomyomatosis and renal angiomyolipoma
- tuberous sclerosis diagnostic criteria
- multiple renal angiomyolipomas
- Dichtewerte Angiomyolipom

 Assoziationen und Differentialdiagnosen zu Angiomyolipom der Niere:
Assoziationen und Differentialdiagnosen zu Angiomyolipom der Niere: