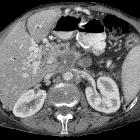
von Hippel Lindau syndrome



















Von Hippel-Lindau (vHL) disease is characterized by the development of numerous benign and malignant tumors in different organs (at least 40 types ) due to mutations in the VHL tumor suppressor gene on chromosome 3.
Epidemiology
The disease is rare with an estimated prevalence of 1:35,000-50,000. Most patients are diagnosed with their first tumor in early adulthood (mean age at diagnosis of initial tumor is 26) .
Clinical presentation
Clinical presentation is varied, depending on the site of disease manifestation (see below). Most commonly these are either within the abdominal cavity or affect the central nervous system.
Pathology
Distribution
Patients may develop some or all of the various lesions which include:
Abdominopelvic
- renal lesions (>67% of patients )
- renal cell carcinomas (RCCs)
- usually of the clear cell type and frequently bilateral
- 70% lifetime risk
- RCCs present at an earlier age (mean = 39 years) in those with vHL
- renal cysts
- can occur in up to 75% of patients
- often tend to be bilateral and multiple
- can be simple, complex or cystic RCC
- renal angiomyolipomas
- renal cell carcinomas (RCCs)
- adrenal
- pheochromocytomas: 25-30% of patients
- extra-adrenal pheochromocytoma / paraganglioma: 15%
- pancreas (may be the earliest manifestation )
- pancreatic cysts: ~40% of patients
- pancreatic neuroendocrine tumors (pNET)
- ~12.5% of patients (range 9-17%)
- usually non-functional
- frequently multiple
- pancreatic serous cystadenoma: ~12.5% of patients (range 9-17%)
- pancreatic adenocarcinoma: rare
- liver
Urogenital
- epididymal cysts
- papillary cystadenoma of the epididymis: ~35% of patients (range 25-60%)
- broad ligament cystadenomas
CNS
- CNS hemangioblastoma(s): occur in ~70% of patients (range 60-80%)
- cerebellar (~60%; range 44-72%)
- spinal cord (~30%; range 13-50%); most commonly in cervical and thoracic cord
- brainstem
- choroid plexus papilloma
Head and neck
- retinal hemangioblastoma(s)
- most common presenting feature, occurring in 45-60% of patients
- vision loss in 35-55% of patients
- endolymphatic sac tumors (ELST)
- occurs in 10-15% of patients
- bilateral in 30% ; considered pathognomonic for vHL
A mnemonic to help remember the features of vHL is: HIPPEL.
Genetics
The disease carries an autosomal dominant inheritance with high expression and penetrance - ~80% of cases occur via this pathway with ~20% arising de novo . It results from the inactivation of VHL, a tumor suppressor gene located on chromosome 3p25.5. However, no mutation is identified in up to 30% of cases.
Classification
VHL can be classified according to clinical phenotypes, and the classification correlates with particular genotypes :
- type 1: low-risk for pheochromocytoma but higher-risk for CNS hemangioblastoma, RCC, pancreatic cyst, and pNET
- type 2A: high-risk for pheochromocytoma; low-risk for RCC
- type 2B: high-risk for pheochromocytoma and RCC
- type 2C: high-risk for pheochromocytoma only
Radiographic features
Please refer to articles on individual lesions for specific imaging characteristics.
Treatment and prognosis
Most lesions from vHL are treatable and surveillance is recommended with various regional guidelines . Some experts advocate routine screening starting in adolescence. Prognosis is poor, with a median survival of ~50 years, with the most common cause of death being RCC and cerebellar hemangioblastomas .
History and etymology
Eugen von Hippel (1867-1939) was a German ophthalmologist who had described a rare disorder of the retina in 1904 and seven years later reported the basis of this disease, named as "angiomatosis of the retina".
Arvid Vilhelm Lindau (1892-1958) was a Swedish pathologist and bacteriologist who described the association between angiomatosis of the retina and hemangioblastomas of the cerebellum and other parts of the CNS and other visceral components of a disease, calling it "angiomatosis of the central nervous system".
In 1964 the disease was renamed Von Hippel-Lindau disease.
Siehe auch:
- Nierenzellkarzinom
- Angiomyolipom der Niere
- Pankreaskarzinom
- Hämangioblastom
- Insulinom
- Phäochromozytom
- Plexuspapillom
- simple Leberzyste
- Tumor des Saccus endolymphaticus
- epididymal cystadenoma in Von Hippel-Lindau disease
- mikrozystisches seröres Zystadenom des Pankreas
- endolymphatic sac tumour in a patient with von Hippel-Lindau disease
und weiter:
- zerebrale Verkalkungen
- intrakranielle Verkalkungen
- Pilozytisches Astrozytom
- Brain stone
- neuroradiologisches Curriculum
- zystische Pankreasläsionen
- autosomal-dominante polyzystische Nierenerkrankung
- Tumoren der hinteren Schädelgrube
- Leukokorie
- Medulläres Schilddrüsenkarzinom
- Phakomatosen
- bilateral renal enlargement
- angiomatosis
- paratestikuläre Läsionen
- Pankreaszyste
- focal hypodense hepatic lesions on non-enhanced CT
- Adenome der Nieren
- syndromes with a vascular component
- papilläres Adenom der Nieren
- serös zystische Neoplasie des Pankreas
- cystic haemangioblastoma of the medulla oblongata in Von Hippel-Lindau syndrome
- hemangioblastoma: von Hippel-Lindau syndrome
- Hämangioblastom der Medulla oblongata
- endolymphatic sac tumour in association with Von Hippel-Lindau disease
- vaskuläre Syndrome

 Assoziationen und Differentialdiagnosen zu Morbus Hippel-Lindau:
Assoziationen und Differentialdiagnosen zu Morbus Hippel-Lindau: