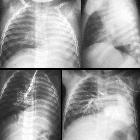
pulmonary hypoplasia


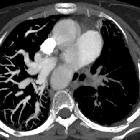


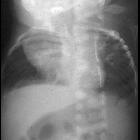















Pulmonary hypoplasia (PH) refers to deficient or incomplete development of parts of the lung. It can develop as a result of a number of other in utero anomalies.
Epidemiology
The true prevalence is not well known (1.4% of all births according to Knox et al. ), but in cases of premature rupture of membranes at 15-28 weeks gestation, the reported prevalence of pulmonary hypoplasia ranges from 9 to 28% .
Pathology
It is characterized by the presence of both bronchi (albeit rudimentary) and alveoli in an under-developed lobe. Both the size and the weight of the lung is reduced.
There are normally four stages of fetal lung development where the pathological process can occur at any level
- embryonic: from conception ~5 week
- pseudoglandular: from ~5-17 week
- canalicular: from ~16- 24 week: this stage may be more affected by oligohydramnios
- terminal sac or alveolar period: from 24 week to term and beyond
Etiology
There are several key factors required for the adequate development of the lung. These are:
- sufficient amniotic fluid volumes
- adequate volume of the thoracic cavity
- normal breathing movement
- normal fluid within the lung
A deficiency in any of these could lead to pulmonary hypoplasia.
Most cases of pulmonary hypoplasia are secondary to other congenital anomalies or pregnancy complications. Some cases however can occur as a primary event .
With secondary causes, it can result from factors directly or indirectly compromising the thoracic space available for lung growth.
Intrathoracic causes include:
- congenital diaphragmatic hernia: most common intrathoracic cause
- extralobar sequestration
- agenesis of the diaphragm
- mediastinal mass(es)/tumor(s)
- decreased pulmonary vascular (arterial) perfusion
Extrathoracic causes include:
- oligohydramnios and its causes
- Potter sequence: fetal renal anomalies
- preterm premature rupture of membranes (PPROM)
- skeletal dysplasias, especially those causing a narrow fetal thorax
- large intra-abdominal mass compressing the thorax
- neuromuscular conditions interfering with fetal breathing
Other associations include:
Radiographic features
Ultrasound
Antenatal ultrasound may show ancillary features such as the presence of oligohydramnios and/or also show any of the causative anomalies.
Several sonographic parameters may give indirect clues as to the presence and extent of pulmonary hypoplasia. Such include:
- fetal lung : head ratio: reduced (ratios <1 usually indicate a poor prognosis)
- fetal chest circumference (or thoracic circumference (TC)) : reduced
(In the case of intra-thoracic causes, both these parameters can be normal)
- thoracic : abdominal circumference ratio <0.6
- femur length : abdominal circumference ratio <0.16
Doppler
Peripheral pulmonary arterial resistance is often increased with pulmonary hypoplasia.
MRI
Fetal MRI may be useful to more accurately calculate lung volumes:
- T1: normal fetal lung is usually low signal on T1; more to be added
- T2: normal fetal long is usually high signal on T2; more to be added
- HASTE: fetuses with pulmonary hypoplasia are thought to have low signal
Treatment and prognosis
The presence or development of pulmonary hypoplasia is often a critical determining feature in fetal survival in context of other potential causative anomalies. Treatment will significantly depend on the presence of underlying/associated anomalies.
Differential diagnosis
In adult cases of unilateral pulmonary hypoplasia, consider conditions associated with a small hemithorax such as:
See also
Siehe auch:
- Scimitar-Syndrom
- Poland-Syndrom
- Pena-Shokeir-Syndrom
- Potter-Sequenz
- Pulmonalatresie
- Swyer-James-Syndrom
- Fryns-Syndrom
- pulmonale Aplasie
- Plazentainsuffizienz
- Neu-Laxova-Syndrom
- Kurzripp-Polydaktylie-Syndrom III Typ LeMarec
- Pena-Shokeir-Syndrom I
- Meckel-Gruber-Syndrom
- Game-Friedman-Paradice-Syndrom
- PAGOD-Syndrom
- Lethales multiples Pterygium-Syndrom Typ II
und weiter:
- Zwerchfellhochstand
- Lungenvenenfehlmündung
- Bauchwandhernien
- kongenitale pulmonale Atemwegsmalformation (CPAM)
- Down-Syndrom
- obstetric curriculum
- Bochdalek'sche Hernie
- Meckel-Syndrom
- Oligohydramnion
- asphyxierende Thoraxdysplasie (Jeune-Syndrom)
- Snowman heart
- Arthrogryposis multiplex congenita
- caudal dysplasia sequence
- kongenitales lobäres Emphysem
- komplette Verschattung Hemithorax
- totale Lungenvenenfehlmündung
- Dextrokardie
- partielle Lungenvenenfehlmündung
- Anhydramnion
- PPROM
- dysencephalia spanchnocystica
- pulmonary venolobar syndrome
- fetal akinesia / hypokinesia sequence
- prolonged rupture of membranes
- pre term premature rupture of membranes
- primary fetal hydrothorax
- fetal cardio thoracic circumference ratio
- Acute Respiratory Distress Syndrome neonatal
- Zwerchfellagenesie

 Assoziationen und Differentialdiagnosen zu Lungenhypoplasie:
Assoziationen und Differentialdiagnosen zu Lungenhypoplasie: